The post Q&A with Dr. Steven Lockley and Mickey Beyer-Clausen: Why “circadian time” will become the foundation of health and wellness appeared first on Global Wellness Institute.
]]>
 Today is the first Circadian Awareness Day! 24 July, 24/7
Today is the first Circadian Awareness Day! 24 July, 24/7
So, we have a very special Q&A with world-renowned circadian science expert Dr. Steven Lockley of Harvard Medical School and CircadianTech pioneer, Timeshifter’s Co-Founder and CEO Mickey Beyer-Clausen on how…
Connecting artificial clock time with our natural “circadian time” will become the foundation of health and wellness.
In this fascinating interview, they discuss:
- How sleep (our cultural obsession) is not the same as the “circadian clock”—and only solutions that have the timing of light at their center can shift or “reset” our circadian rhythms.
- How our modern world is a circadian nightmare. The future? Solutions that maintain or “reset” our circadian rhythms, a revolution not only for shift workers and jet-lagged travelers but for ALL of us, with our always-on, Zoom-at-5 AM, digital lives.
- How circadian science will transform medicine, with drugs, treatments and vaccines timed to your circadian cycle for maximum efficacy and safety.
- How the future is “circadian wellness”: When is the best time to do that high-intensity workout, eat that particular food, or have that important meeting.
Every July 24 is Circadian Awareness Day, which shines a light on the extraordinary effects our 24/7 circadian rhythms have on our safety, performance and health. LEARN MORE

Dr. Steven W. Lockley, BSc, PhD, is a world-renowned sleep and circadian neuroscientist. He is an associate professor of medicine, Harvard Medical School; a neuroscientist at the Division of Sleep Medicine, Brigham and Women’s Hospital; and the co-founder and chief scientist at CircadianTech pioneer Timeshifter. Dr. Lockley has spent 25 years studying ways to reset the circadian clock and works with clients such as NASA and Formula 1’s elite.

Mickey Beyer-Clausen is a Danish-born, New York-based entrepreneur with a track record of building genre-defining companies. Mickey is the co-founder and CEO of Timeshifter—a circadian science company translating sleep and circadian neuroscience into apps to improve the safety, health and performance for billions of people. Before Timeshifter, Beyer-Clausen co-founded several other businesses, including Trunk Archive, Ascio Technologies and Happiness Foundation.
Both will keynote at the next Global Wellness Summit (November 30–December 3) in Boston, where they’ll share more mind-blowing insight on how circadian neuroscience will drive the future of health and wellness.
I) People are obsessed with sleep, but it’s NOT the same as the circadian clock
McGroarty, GWI VP of research: One of our top wellness trends for 2020 was that the wellness world would shift from their obsession with “sleep” (and the storm of “sleep solutions”) and focus on what matters more: managing circadian rhythms. With Dr. Lockley’s incredible scientific guidance, we tried to explain that ANY solution that claims to “reset” circadian rhythms must have the TIMING of light at its center. We tried, but confusion still reigns. Dr. Lockley, can you “nutshell” the difference between the “circadian clock” and “sleep”? And why it matters?
Dr. Lockley: The confusion is understandable because these are challenging concepts. The circadian system controls the timing of many bodily systems, of which sleep is just one. The circadian (24-hour) clock also controls the timing of many rhythmic functions, including many hormones, lipid and glucose metabolism, immune function, reproductive hormones, bone metabolism, mood and performance, and many others. The circadian system is more wide-reaching than sleep: Sleep is just one output of that central clock. You can think of the clock in the brain as the conductor of an orchestra, keeping the individual members of the orchestra (different organs and functions in the body and brain) in synch. There are clocks in the heart, lungs, kidneys, ovaries and many other cells that can keep their own time but look to the conductor for overall timing. Another analogy: Like that old analog watch on your wrist, there are different hands of the clock that the central clockwork controls. So, think of sleep, metabolism, hormones and immune health as different hands controlled by that central circadian clock in your brain.
What is KEY is that if you want to control the timing of the circadian clock or reset a disrupted clock, you need to develop interventions that have the type and timing of light at the center. Light is the major time cue that synchronizes our circadian rhythms, and light is the solution to reset them. By correcting the timing of the circadian clock, you automatically correct the timing of the systems the clock controls, bringing them all into line to work as efficiently as possible. Circadian disruption is quite common—many of us experience it—and science-based solutions to address the underlying circadian disorders are needed.
The daily solar light-dark cycle is the crucial time cue that resets our clocks every day; if you don’t take in light and dark (like blind people), you can’t reset your clock. Man-made light can both help and hinder this process, depending on when you see it: Electric light after dusk is potentially disruptive but can supplement daylight in the day (or replace daylight if a night-shift worker). Regular, consistent light cues (and therefore wake/sleep schedules, as wake equals light and sleep equals dark) are the pillars of circadian health, but it’s also personal: We all have a slightly different clock time or chronotype. “Early birds” have a clock that cycles faster, and they typically feel better early in the day; “night owls’” clocks cycle more slowly, and they tend to feel better later in the day. Individual chronotypes have many real-world effects because they impact how you line up with time and the world: essentially, when you work best, digest food most efficiently, sleep the longest, etc.

II) The modern world is a circadian ‘lightmare’
McGroarty: Why are we in such a circadian disruption crisis now?
Dr. Lockley: Think about all the disruptions to our circadian clock that have been unleashed in the last 100 years, making us no longer attuned to the natural light/dark cycle. With electric lights, we override that cycle, exposing ourselves to light in the evening and overnight. Jet travel means hopping to new time zones so fast that our clock can’t keep up, causing jet lag. Shiftwork—only possible since the widespread introduction of artificial light—has surged, causing extreme “clock” misalignments. And in a digital, global world, we all expose our eyes to the alerting “blue-enriched” light emitted by electronic devices. We have all become shift workers to some extent, with always-on work and Zoom calls. Those early starts or late nights are “shiftwork” in a way, just less extreme, but can still have damaging effects on circadian rhythms and the myriad systems it controls. Our modern world conspires to disrupt the circadian system, and when those systems are out of sync for years, you not only see sleep problems but higher rates of heart disease, diabetes, depression and some cancers. This is why solutions that can maintain or “reset” our circadian clocks to the right time will be the future of medicine and wellness.
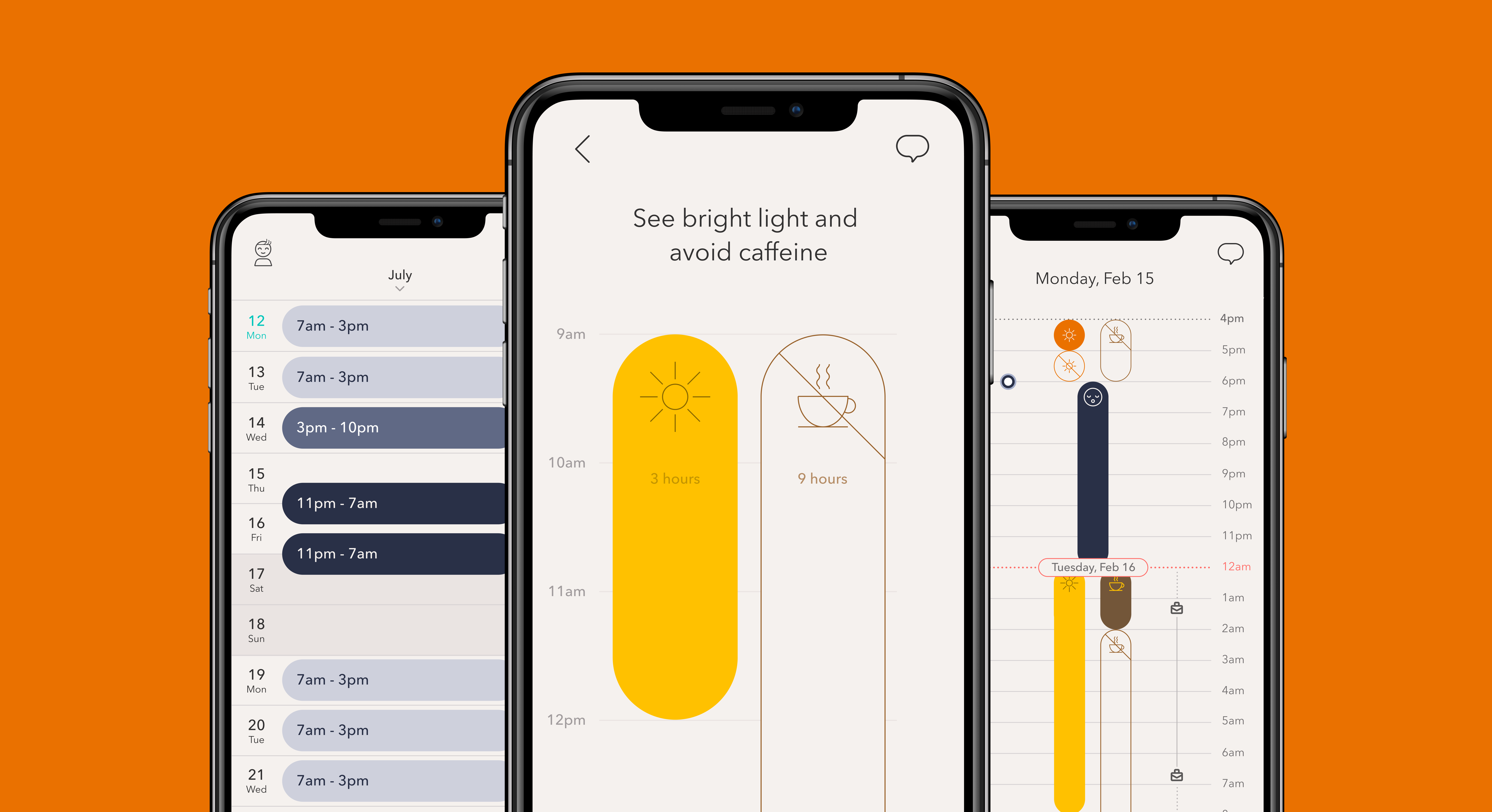
III) How “time-shifting” solutions can eliminate jet lag and improve the health of shiftworkers
McGroarty: And that’s where Timeshifter comes in. First, you launched a jet-lag app, which “shifts” people to new time zones by telling them exactly when to take in dark and light and to sleep (and not). I used it on a trip to Singapore (yes, I wore sunglasses in airports at night), and if you comply, it’s a miracle: no jet lag. Now, you’re expanding into a circadian, “time-shifting” solution for shift workers. Tell me why that’s so important?
Beyer-Clausen: Jet lag was the natural place for us to start, and after we launched that app in 2018, we saw a boom in people using it. COVID temporarily disrupted travel and that adoption, but now it’s coming back. We’ve analyzed surveys from more than 80,000 users, and if you don’t follow the app’s advice, you’re six times more likely to experience severe jet lag and 17 times more likely to experience very severe jet lag! But Timeshifter isn’t just a jet-lag app; our plan has always been to solve other large, previously unsolved circadian-based problems.
Next up is shift work, a disruptive circadian misalignment problem leading to huge worker safety, productivity, and physical and mental health issues. With almost 700 million people (20% of the US workforce) working shifts and struggling with irregular work schedules, we can’t continue to ignore the many negative consequences it causes. Shift work and irregular hours are prevalent in many industries, including manufacturing, construction, mining, security, hospitality, warehousing, delivery and transportation. The extent of the problems associated with shiftwork makes it an exciting problem for us to solve because it will make such a huge difference in people’s quality of life, productivity, safety and health.

ift work was a more challenging problem for us to solve than jet lag, which tends to be an infrequent experience. Both involve severe disruptions in the light-dark exposure cycle, but for shift workers, the problem is often continuous and chronic. So, the new app gives advice on when that worker should take in light and dark (and their optimal sleep times) in a continuous way. We also had to factor in people’s daily realities (you have to pick up your kids at school, which affects when we can ask you to sleep, for example), so we built in the ability to add personal constraints in addition to our “practicality filters” that ensures our advice is easy to follow in the “real world.” With every solution we build, we want to rigorously translate the science into an experience that’s highly intuitive and easy to use.
IV) With always-on work, and whacked out light exposure, we ALL need circadian “resetting”
McGroarty: But what about circadian solutions for “regular” people like me? With the Internet killing the divide between life and work (goodbye 9-to-5), which was further killed by work-from-home and Zoom calls that happen at 5 AM and midnight the same day, don’t we ALL need constant “time-shifting” and circadian resetting?
Dr. Lockley: Absolutely: Circadian disruption is a continuum, and these problems run all through society, from people who do the same thing every day to extreme shift work. The more variability, or “wobble” in behavior, you have in your circadian clock day-to-day (erratic sleep/wake times, light/dark exposure), the more health and productivity problems you’re going to have.
Beyer-Clausen: There’s huge potential for us and others to build tools that help everyday people manage their circadian clock far more effectively. If you use science to estimate where people are at in their circadian cycle, apps can help you TIME your life far better: When is the best circadian time for individuals in Singapore and LA to Zoom or how to make sure your brain and body are ready when you need to be at your best.
There are so many use cases. Athletes want to perform when their body is at its most alert, energized state, but running a marathon at 9 AM is radically different than playing a basketball game at 8 PM. So, we’re working with Olympic athletes to match performance time to peak circadian time.
Ten years ago, sleep was not a cultural priority, and people bragged about not sleeping. Now, it’s a half-trillion-dollar economy. Expect circadian science to go mainstream in the next few years and the circadian economy to eventually overtake the sleep economy. The future is connecting artificial clock time with “natural time”—your individual circadian clock. It’s about making “circadian time” every bit as important as clock time—something just as visible to you on your watch—so you know what’s happening in your body, can time activities in your life better, and even proactively “shift” your circadian clock to tackle jet lag, manage changing work schedules, be at your best when you need to perform, or increase the antibodies stimulated by your vaccine.
V) Circadian science will transform many industries, from the timing of medicine to sunglasses
McGroarty: Any other major circadian issues that need fixing? What’s ahead in the future?

Beyer-Clausen: Here is one example of an overlooked problem that could easily be turned into an opportunity: The multibillion-dollar sunglasses industry has so far focused on enhancing color and contrast so their customers can see more detail but often forget that their lenses also alter the quality of light the eye receives to reset the circadian clock or alert the brain. Who wants their sunglasses to tell their brain that it’s night during the day, making them sleepy exactly when they don’t want to be or tell their brain it’s day in the evening, making them alert when they want to prepare for sleep?
Just like with our ears which control hearing and balance, our eyes have two separate functions: One is to see our surroundings (that’s all we have thought about until now), but the eyes have a second, completely separate system sending light and dark cues from special cells in the eyes directly to our circadian clock, telling the brain if it’s day or night. If we’re wearing sunglasses that don’t let in the right spectrum or intensity of light, you’re messing with the circadian clock. We need “circadian-enhanced lenses” that help us both see well and inform the brain what time it is—an enormous new opportunity for the industry. This would be great in our daily lives but also enable an even better time-shifting experience when we travel or work at night shifts.
Dr. Lockley: And the current “blue-light-blocking” glasses approach can be overly simplistic and unscientific: Blocking blue light is one component, but other wavelengths of light at night negatively affect the circadian system and need to be addressed.
Dr. Lockley: In the not-too-distant future, we will be applying circadian science in medicine, which will take many forms and have a massive impact. Right now, medicine all revolves around clock-time, not an individual’s circadian time, but we see differences of up to nine hours in the timing of circadian clocks between individuals living in the same time zone! You and I are given drugs, treatments and vaccines at the same clock-time even though our circadian rhythms might be very different. It might be better for you to take that morning pill at 7 AM, but better for me to take it at 10 AM to get the best effects or fewer side effects. We know, for example, that different vaccines work better at different times of the day and are likely to work even better if we timed them to individual circadian times. In another example, you and I might get a lab test at the same time, but you’re an early bird, I’m a night owl, and the results will be different and need to be interpreted differently. We’ve known for over 20 years that with certain chemotherapies, the timing matters and can have a big impact on toxicity and even mortality rates (there have been encouraging clinical trials, but bigger ones are needed).
Beyer-Clausen: Medicine needs to incorporate circadian timing as a factor in clinical trials for drugs because the majority of medications likely have a circadian element in terms of maximum efficacy and also toxicity. If you take drugs at the right time, you might be able to use less for the same benefit. So, in the future, we will have clinical standards governed by circadian time, and you will be able to measure your circadian rhythms in the doctor’s office, just like your blood pressure, to inform advice at the right time for you. Clinics might say, however, that it will be too difficult to get everyone their ideal “circadian” appointment time. But with Timeshifter, if a patient has a noon chemotherapy or vaccine appointment, we can shift their circadian clock to match that appointment time. We don’t need to shift the medical system, just the patient. We’re looking for pharma partners to collaborate with us to understand COVID vaccine timing, for example, because if you could change the percentage efficacy even by a small amount by delivering vaccines at the optimal time, you could have an enormous impact on world health.
Once we measure and model circadian rhythm timing more routinely, we’re going to find that so many medical interventions have a circadian component—for things we don’t even realize yet. The new era of circadian medicine will become a routine part of your healthcare management, and in terms of prevention, it’s going to have a revolutionary effect: Getting the timing of medicine right will improve the health of billions of people.
VI) Wellness–from when to exercise, eat or sleep–needs to embrace circadian timing
McGroarty: What about the timing of “wellness”?
Beyer-Clausen: Every aspect of health and wellness is governed by the circadian clock. Circadian rhythm measurement and advice can tell you when it’s a better or worse time for everything from that high-intensity workout to eating a particular food.
Dr. Lockley: There are so many wearables tracking all kinds of data, and what we need to do is put the timing of that data at the very center of health tracking. It sounds biased, but justifiably so, given the ubiquity of circadian rhythms on our biology, organs and cells. There’s a lot of promise in harvesting the wealth of biometric data out there to detect and optimize circadian rhythms if used correctly. Wellness depends on timing for eating, sleeping, and exercising, but at the moment, circadian timing is not adequately accounted for. When it is, the health benefits will be even greater.
McGroarty: Whenever I talk to you, my mind reels. I’ve learned that with health and wellness, “timing is everything”—and I’m now pining for a watch that tells my “circadian time” and pondering my defective designer sunglasses. Thank you!
ADD A COMMENT BELOW
The post Q&A with Dr. Steven Lockley and Mickey Beyer-Clausen: Why “circadian time” will become the foundation of health and wellness appeared first on Global Wellness Institute.
]]>The post Q&A with Spa Industry Icon Sue Harmsworth: Why “Wellness” Needs New Definitions appeared first on Global Wellness Institute.
]]>

Sue Harmsworth, spa industry visionary
Sue Harmsworth needs little introduction: She has spent five decades shaping the global spa, global wellness and beauty industries (responsible for designing 500+ spas in 65 countries), and her services were honored by Queen Elizabeth the Second. She founded the global brand ESPA in 1993, which she sold in 2017; is founder of Sue Harmsworth Ltd, which advises owners and private equity firms on creating wellness destinations; and she sits on various boards, from Forbes to the Global Wellness Institute (GWI).
In this edition, Harmsworth discusses:
- Why the term “wellness” has reached near meaninglessness—and how we need new distinctions
- How integrative wellness resorts—which marry “serious” and “light” wellness—are the future but will require a whole new kind of operator
- How the pandemic experience is fueling consumer desire for wellness real estate—and how more affordable communities are rising
- Why the spa practitioners of the future must be trained better and deeper
- What investment bet she would place in wellness

Beth McGroarty, GWI VP of research and forecasting: In your recent master class with us, you discussed how the term “wellness” has become so oversaturated and overstretched it’s reaching the point of meaninglessness. And that the time is now to make new distinctions. Talk more about this problem, what new distinctions need to be made, and why.
Harmsworth: I’m starting to hate the word wellness (laughing) because it’s become so generic it’s utterly confusing the consumer. Everything is labeled “wellness”: You go to the supermarket, and you’re overwhelmed. We need new terms and definitions—and as an industry, we don’t challenge ourselves enough to be clear with consumers. It’s becoming a real issue with social media moving so fast and so much copying going on.
The history of wellness and spa—and the regional differences—add to the confusion. What we think of as “wellness”—all the ancient medical traditions from TCM to Ayurveda; amazing, centuries-old “kurs” at European health farms; the hydrothermal piece; advanced massage techniques—these existed forever before modern “wellness” was born in the spa industry in the 90s.
As the spa industry took off, the word and concept became confusing, and it has to do with what the US means by it versus the rest of the world. In the US, every beauty salon, or every two treatment rooms by a pool, suddenly became a “spa”—not what I, as a European, would call one. When the spa movement became powerful in the 90s, stress was the overwhelming focus. The world was changing: Women were going back into the workforce, flying constantly became the norm, and technology was taking over the world. Stress was the huge issue, and most spas were built for relaxation—from massages to meditation. What I would call “light wellness”—with no negative connotations.
But now, we have a much more complex set of modalities and advanced practitioners at wellness destinations. We have fitness/sports, a much more serious nutrition and microbiome piece, spa, complementary medicine, and beauty—but aesthetics as in both medicine/machines and more non-invasive approaches. And we have more medical or “serious” wellness. But there can be confusion around “medical wellness” for consumers: They may think it means traditional allopathic medicine and ask, why would I go to an expensive resort when I can do the same things with a specialist? The future of medicine at destinations is functional medicine and preventative, advanced testing and diagnostics: whether hormone analysis, 3D scanning analyzing bone density, muscle mass and visceral fat, or microbiome and nutrition testing. All to create a personalized health plan.
So, you have “light wellness,” which spas and hospitality destinations have excelled at. You have medical or “serious” wellness, but it’s different this time around: It’s preventative, functional medicine and diagnostics. That’s why I’m so keen on new definitions and distinctions: “Wellness” is too imprecise to mean anything. People have got to focus on what their consumers want and get clear about what they’re delivering.

McGroarty: I know you’re working on some big integrative wellness destinations—and you believe that’s the future. Why?
Harmsworth: It’s absolutely the future, with all the lifestyle diseases hitting us so hard, and I’m working on properties now that bring everything together: functional medicine and diagnostics, an aesthetics clinic, and all the traditional wellness, from complementary medicine to fitness to serious meditation (with Buddhist monks or TCM). Mental and cognitive health will be huge coming out of the pandemic, with depression and anxiety having risen exponentially since COVID and now affecting a third of the population globally.
One reason the functional medicine and diagnostics piece is so key is that with all the wonderful destinations focusing on Asian traditions (the Indian, Thai or Balinese approaches), people weren’t given concrete results. When you’ve gone to medical-wellness clinics in Germany or Austria, they do advanced testing (whether hormones or vitamin deficiencies) on intake, and when you leave, you do them again. You can see the results. It seems crazy, but you really can significantly impact your blood pressure or cholesterol in one week. What I want to do—and it’s the future—is to be able to program individuals on a personalized plan with a very full set of stats so that they can see their results over time.
McGroarty: Operators and investors have struggled to get even the ROI of a spa in a hotel project. What needs to change to pull off these far more ambitious integrative wellness destinations?
Harmsworth: First, it’s going to take an entirely new operating model and type of operator. There’s lots of great operators on the clinic side; I could run through some of the big names from Lanserhof to SHA, but they’re not as integrated as I think the future will be, and I don’t think there’s an operator out there right now with this forward-thinking, bring-it-all-together approach.
We need to remember that, historically, spas—outside the US—haven’t been particularly profitable. That’s because the hotel model is to view every department as a completely standalone profit center, so they isolate a spa’s costs and revenues (staffing, utilities, laundry, etc.), so it often doesn’t show a good ROI—and also, unless you have a hotelier or developer who really gets it, they haven’t been spending the capital on spas that would let them actually see the ROI.
In the US, developers who’ve been building shopping malls and condos typically don’t understand spas at all: they think narrowly in terms of square-foot return on investment. But this will change: The hospitality industry is recognizing the importance of health and wellness to the consumer, and that means everything: nutrition/menus, lighting, air and water quality, sleep quality, a great spa/wellness center.
What operators need to learn is that you’ve got to turn the model on its head. It’s much easier to make an integrative wellness resort profitable because the medical diagnostics and medical-aesthetics areas (while the practitioners are much more expensive) can be hugely profitable, far more so than any spa. Integrative wellness resorts will have a whole different profit and loss model than the departmental formulas of hotels: You will look at the bottom-line profit across all departments, where all is wellness (rooms, F&B, spa, medical services, aesthetics, etc.) It’s one pot; they will be very profitable, even if there is a loss leader.
Second, we need to build destinations broad enough so the consumer can do different things at different times. Most people that want a vacation want wellness: to eat right; to have stimulating, healthy things for kids (cooking classes, foraging, sailing—not some boring Kids Club)—but they want to relax, have a few drinks, have fun. On the other extreme, some people need much more: You’ve had cancer or put on 20 pounds, etc. You want the strictness and deeper functional medicine of a medical-wellness environment to do something more intensive, often alone. And then desires fall everywhere in-between. More healthy people now want to assess their life once or twice a year for preventative reasons: to be the best at every stage of their life, to pick up the little things before the big things happen. Like me, they start seeking prevention in their 20s and 30s. This is all much broader than what’s come before. And if you can bring it all together without confusion, it’s going to make money. For sure.
This is a design issue and one I’m right in the middle of with my projects. Most medical spas have been quite small (say, 50 bedrooms). To achieve this new integrative model, the resorts are going to have to be bigger, and the whole nature piece will be enormous: the great outdoors, a warm enough climate, and the quality of the air. It’s about creating a place that can have paths that run from fun and families to the more serious, preventative stuff.
Third, it will be much easier to make an integrative wellness resort stack up financially with the residential component.
I’m working on the Amaala project on Saudi Arabia’s Red Sea, spearheaded by their ruler, Prince Mohammad bin Salman bin Abdulaziz Al-Saud, a wellness resort and community at the ultra-high-net-worth end. It’s set on 435 miles of coastline and will integrate everything from advanced medicine to comprehensive wellness approaches—and many of the main wellness brands will be there. It’s an interesting example of designing for different needs and guests, with both an integrative wellness resort for adults and another for families.

McGroarty: There’s no greater expert—give me a prediction for the future of spas.
The really good spas where the therapists and treatments are good, the hardware and thermal areas are good, the design and flow are good, the air quality and infection control are good—they will start to take on even more approaches from the “light wellness” side.
However, in the future, spa therapists and practitioners are going to have to be much better trained with deeper skills. They need a much broader knowledge set to be able to deal with all the things increasingly coming their way. They’re bombarded by clients with more serious issues (diabetes, cancer, heart disease, depression and grief): The majority that walk in now have some kind of contraindication. This is why I’m so strong on what we’re doing in the UK with the training ruling bodies, putting modules together so that well-qualified therapists (we call them level 3 or 4 here) can keep adding modules (whether cancer or nutrition training) so they can deliver more “wellness” than just massages or facials, be empowered to deal with the day-to-day realities they see, and be set on a career path of constant skill-upgrading. The spas that will take it to the next level will focus on training in a much more intense way.
McGroarty: The pandemic seems to have given wellness real estate and communities new momentum. What do you see in the future?
COVID has obviously woken all of us up to working from home, and this ongoing reality will drive real growth in wellness real estate and communities—and in more affordable projects. Look at me: I haven’t budged from my second home in Tenerife since October. This is the longest I’ve been in one place in 40 years (no planes), and I’ve worked just as efficiently from here as anywhere. It’s completely changed my thinking: I love being in one beautiful place, and I’ll never fly the way I did before. All those businesspeople flying week after week; that’s all going to slow way down and have to be justified.
Since the pandemic, people are spending a lot—or all of—their time in their second homes. More people will choose a wellness community as the primary (or near-primary) residence, and maybe they’ll have a pied-à-terre in the city and go in one or two days.
This will drive more affordable wellness communities. I’m working on a wellness real estate project now (still at the concept stage) where you go from the most expensive villa at $1 million to artisan homes down to $300,000—that’s relatively affordable. It will be an interesting community: They will grow everything themselves and have their own Waldorf school for the kids.

Another multisite project I’m working on is also affordable because the cost of the real estate makes the difference (and this is purely real estate, with no hotel). I can’t give much away, but it has the obvious things you would expect—yes, yoga, yes, a spa—but it’s really much more about an entire lifestyle of wellbeing. We will see more of that.
I’ve always said, don’t put me in some place with a bunch of old people—and the way forward is multigenerational wellness communities.
It’s all so interesting how desires are shifting: Even people with lots of money, while they want to buy in a better, more naturally beautiful location, don’t necessarily want to buy bigger. I’m working with a very wealthy New York developer (third-generation real estate company) on a Costa Rican wellness community. He doesn’t want a bigger villa; he wants a truly sustainable villa for his kids—a whole different, healthier way of living. He’ll have to go to New York sometimes but not often.
McGroarty: You’re an investor in wellness. Name a segment you would place a future bet on.
Harmsworth: I’ve talked about the future for integrative wellness destinations, with more serious, preventative functional medicine and diagnostics. People go to “serious” wellness resorts, do a battery of tests/scans, come out pumped up to change their lives, and—it’s human nature—in a few months, they’ve fallen off the wagon. I think a crucial future of the tech piece is both advanced diagnostics and anchoring people to the site for ongoing monitoring and follow-up—using AI and “tele” models. I’d invest there. (As an aside, I can’t stand all the mindfulness technology; it doesn’t work for me.)
I also think you have a huge singles market coming up (people divorced, widowed, that don’t want to get married or remarried), so hospitality models that combine comprehensive wellness with fun and the social piece will rise.
ADD A COMMENT BELOW
The post Q&A with Spa Industry Icon Sue Harmsworth: Why “Wellness” Needs New Definitions appeared first on Global Wellness Institute.
]]>The post Q&A with Dr. Shoshana Ungerleider: What Has the Pandemic Taught Us About Wellness, Death and Dying appeared first on Global Wellness Institute.
]]>

Shoshana Ungerleider, MD, founder of the End Well project
Dr. Shoshana Ungerleider is an award-winning physician, writer and producer—and founder of End Well, a series of events and a media platform focused on transforming the end of life into a human-centered experience. She is a leading voice in healthcare who regularly appears on CNN, MSNBC and CBS News and is the executive producer of two Academy Award-nominated documentaries about the end-of-life experience: Extremis and End Game. Her most recent documentary is about the life of Robin Williams, Robin’s Wish. She was a keynote speaker at the 2020 Global Wellness Summit.
In this edition, the GWI’s Beth McGroarty asks:
- What has the pandemic revealed about what most needs fixing in our culture around health, wellness, death and dying?
- Is there tension between the “dying well” movement and the wellness world’s obsession with longevity and anti-aging?
- What can any wellness business do to embrace the “end well” movement?
- What is the future of “dying well”? Where do psychedelics fit?

Beth McGroarty, GWI VP of research and forecasting: 2.7+ million global deaths. Who could have predicted exactly one year ago that our world would be gripped by so much grief, trauma and dying? What has this year revealed about what most needs fixing in our culture around death and dying—and in health and wellness?
Dr. Ungerleider: I will speak from my experience: I see a significant shift in the conversation around mortality among my friends, colleagues and relatives. People have realized, no matter your age, that tomorrow is never a given: You can be impacted by serious illness and death at any stage of life.
And, I think to some degree, every single person in the world is grieving right now. Not everyone has lost a loved one, of course, but we’re all feeling this collective loss of life, and this experience of truly collective grief is new for modern society.
The pandemic has also shined a light on the hidden world of caregivers, both informal (untrained and unpaid) family caregivers and our frontline healthcare workers. We’ve all learned something about what it’s like to be on the frontlines during a pandemic and risk your life every single day.
Our workforce of clinicians has been dramatically traumatized by this experience: from not having the PPE to not having the mental health support when we need it at our hospitals. One year out, the professional burnout is intense, and it’s hard to even think about the number of people who may leave medicine altogether—which is hugely problematic for everyone.
So many of my clinician colleagues are now really suffering and grieving but don’t have the time or space to experience it or get support because they’re so busy taking care of patients. A key lesson we’ve learned: We need to do far more to treat our frontline healthcare workers as human beings and create the services/support that they need to continue doing their job.
When I think about all the ways this last year has unfolded for people, I don’t think we even have the vocabulary that could hold the weight of what this has truly been.

One issue that the pandemic has cracked wide open is that every medical clinician needs to be trained in palliative care. Palliative care is a team-based medical specialty, usually consisting of a nurse, doctor, social worker and chaplain who think holistically about quality of life and reduction of suffering for people and their families facing a life-limiting illness.
Because of the speed and severity with which COVID-19 takes hold of people, it made it painfully clear that providers in the emergency room and ICU (and other specialists) aren’t always trained in having conversations with people about their goals of care. If it’s not clear whether a patient may survive a hospitalization, they may need to communicate things like: If we have to put you on a machine to help you breathe, would you still want that type of intervention if it meant you may not be able to come off that machine? And, identify what people actually want based on their goals and values for however long they have.
Medicine is always poised to offer more treatment because that’s, frankly, how the healthcare system is set up, and some perverse incentives are at play. The culture of medicine means that, by default, you will receive the most aggressive, invasive treatment, no matter how old or sick you are, and sometimes even if it won’t help you. You will end up in the ICU hooked up to tubes and machines unless you opt out loudly or have someone in your corner advocating for you to receive something different.
COVID-19 made it even clearer that people of all ages need to talk openly about what they want and put it in writing. And that every single person in medicine needs to be trained on how to have honest conversations with patients and families to get at what they truly want from their care.
The “end-of-life” experience: Serious illness care, caregiving, the emotional/psychological aspects of the death and dying process, as well as grief and bereavement, are all part of a human journey that every person experiences in their lives. We need to make this experience better for people at every single level.
The pandemic also revealed—in real time—that we have a radically unjust healthcare system. Black and brown communities suffer a disproportionate burden of disease; they have less access to medical care and representation within the system. These, and a number of other factors, led to far greater rates of COVID-19 hospitalization and death, especially because of increased rates of obesity and other comorbidities such as high blood pressure and diabetes. This was further exacerbated by communities of color being more likely to be essential workers who don’t have the ability to take time off work if they are sick. The racial inequities at every level—from access to healthcare to preventive wellness throughout life to end-of-life care—need to be addressed in a very explicit and real way.
What we learned this year: We need to have many very hard conversations, starting with access to healthcare and wellness is systemically racist.
McGroarty: What personally made you interested in rewriting the end-of-life experience?
Dr. Ungerleider: When I was just out of medical school, I spent many months training in the ICU. I was utterly shocked by the amount of suffering I saw for people at the end of their lives—people of every age, but especially older people, who were often very frail, with end-stage cancer or organ failure, spending their final moments hooked up to machines and surrounded by strangers, hidden away from people they loved. I would look into their eyes and see tears and so much pain.
And I thought, my goodness, did this person choose this trajectory? How did they end up here? Nobody ever asked them, if time is short, how do you want to spend that time? What are your goals and values? What does a good day look like for you? I guarantee that the vast majority (if asked) would not have said, with IVs placed all over my body and sedated—hidden away from everyone in my life.
 So, I started End Well, thinking, wouldn’t it be amazing if we had a TED-style conference where we invited people from many disciplines—design, tech, philanthropy, the arts, education, law, policy, healthcare, patients, and caregivers—to really talk about their experiences and learn from who’s doing the great work on the ground, so we could create new solutions, services and products that make a more humane end-of-life experience accessible for more people.
So, I started End Well, thinking, wouldn’t it be amazing if we had a TED-style conference where we invited people from many disciplines—design, tech, philanthropy, the arts, education, law, policy, healthcare, patients, and caregivers—to really talk about their experiences and learn from who’s doing the great work on the ground, so we could create new solutions, services and products that make a more humane end-of-life experience accessible for more people.
It turned into a global movement, transforming the end of life into something more human-centered, finally seeing the end of life as part of life.
We then created a media platform (written and video content), and even though we’re a tiny little team with no media or content delivery experience, we get tens of millions of views organically—evidence that this is a relevant issue for people.
McGroarty: The dying well movement is accelerating and lives under the “wellness umbrella.” At the same time, the wellness world leads with a strong message around anti-aging, “do this and live forever”—in biohacker circles, even “curing death.” What’s the impact of this “wellness paradox” on our culture?
Dr. Ungerleider: We just did a Clubhouse panel (with the founders of Wired magazine and TEDMED) on this exact topic, one that fascinates me personally. I don’t think there is any paradox between the “dying well” and the longevity focus in health and wellness. We’re all after the same thing: How can I live as well as possible as long as possible? It would be amazing if people could live longer, and there is amazing research into how cells age over time.
But it’s not just about living longer; it’s about having a good quality of life for those years, being able to have experiences that are meaningful and bring you joy. Until scientists figure out how to keep us alive, living well, and in a sustainable way for the Earth, there are many millions of people impacted, right now, by illnesses that modern medicine cannot cure—so the focus also needs to be on helping people end well. We can all unite around this: Live long, live well, and die well.
The wellness world needs to embrace that having a relationship with your own mortality is a key part of wellbeing; grasping that your life will end allows you to live better every day. You pay attention to life’s small miracles: the sunset, that hummingbird visiting your window during the pandemic.
 McGroarty: Most wellness businesses are, of course, not in the end-of-life space. What can they tangibly do to support this movement?
McGroarty: Most wellness businesses are, of course, not in the end-of-life space. What can they tangibly do to support this movement?
Dr. Ungerleider: Every business (big or small) can be a change-maker by talking openly about what employees are facing (are they caregivers? facing grief and loss?) and creating a safe, supportive space in the workplace, whether that’s in person or remote. It starts with the C-level leadership saying this is important and acting accordingly. There are so many programs and services you can embrace: providing caregivers paid leave, helping them get trained to be better caregivers at home, connecting people to bereavement support options for those facing grief.
We need to think differently about workplace wellness: It’s not just about yoga, meditation and healthy food. There are so many day-to-day life issues to address, and the end-of-life piece gets missed because it’s hard and not sexy. But it’s so incredibly important for employees.
McGroarty: Any predictions for the future of the “end well” movement? How about the eye-opening research on psychedelics’ impact on end-of-life distress?
Dr. Ungerleider: The early data I’m seeing in the psychedelic space is really encouraging.
What we know: The use of psilocybin, for example, under very strict guidance in a therapeutic setting does significantly reduce existential distress for people facing a life-limiting illness. And with very few side effects and a durable effect, meaning it lasts a long time: Johns Hopkins University found that it continued to reduce anxiety and depression for 80% of people with a life-threatening illness after six months.
We don’t have any modern, FDA-approved medications that achieve that effect. Nor do we recognize existential suffering as we should: We sedate people who exhibit symptoms that are very normal when people approach end of life. So, if psychedelics can reduce suffering with little risk of negative side effects, we need more studies that demonstrate this—and then we need to shift our thinking and make them more accessible as a therapeutic option.
I’m so data-driven; I’m not prone to making predictions. But I can tell you that in 20 years, my hope is that I don’t have to do this work anymore—that I can shut End Well’s doors—because we’ve sorted out how to treat people thoughtfully at the end of their life, and it’s just part of normal care that we provide to people.
We’ve learned some terrible lessons this past year. I’m hopeful we can grow from this experience, and everything we’ve learned will help us move forward toward making ending well possible for all.
We want to hear from you
One year into the pandemic, what do you think it has revealed about what most needs ‘fixing’ in health and wellness?
The post Q&A with Dr. Shoshana Ungerleider: What Has the Pandemic Taught Us About Wellness, Death and Dying appeared first on Global Wellness Institute.
]]>The post Q&A with Victor Brick: Why the Wellness Pie Has Never Been Bigger appeared first on Global Wellness Institute.
]]>

C. Victor Brick, CEO of Planet Fitness Growth Partners and the founder of the John W. Brick Mental Health Foundation, on the Future of Wellness.
C. Victor Brick has 35 years of success in the fitness industry and is CEO of Planet Fitness Growth Partners (PFGP), the largest privately owned Planet Fitness franchise with 80+ clubs in the US and Australia. He’s chairman of the John W. Brick Mental Health Foundation and a Global Wellness Summit Advisory Board member.
Victor Brick predicts:

- Nearly endless opportunity for wellness, as it becomes part of the healthcare delivery system
- Mental wellness as the industry growth-driver
- A limit to the digital fitness boom
- A new era of inclusivity/affordability, as the “other 80%” are now a huge market opportunity
- A new focus on resilience and positive stress
Beth McGroarty, VP, Research & Forecasting, GWI: So much has been written—so many surveys done—on how the pandemic has made wellness more important to people. What’s your take on the future of wellness?
Brick: This is the most earth-shattering event since World War 2, and it will affect every aspect of civilization for the foreseeable future. It’s creating a whole new economy and mentality, and I believe there is nearly endless opportunity for wellness if we have the courage to push wellness to go where it belongs: as part of the healthcare delivery system.
The pandemic revealed that everything we’ve been saying for years about prevention is painfully true. It’s our time; it’s a classic case of never wasting a crisis. Wellness will move to the true mainstream, and once it’s mainstream, everything changes: The medical world, governments and employers will all invest in “more wellness.”
McGroarty: Why has healthcare resisted integrating preventative wellness approaches for so very long?
Brick: The world operates in silos: The medical world, the political world and the wellness world all operate in their own silos, and they’re totally different cultures. There’s a complete lack of consensus on things like how to deal with a pandemic because we have not worked together. Even within the wellness community, everyone is in their own silo: The fitness community, the travel community and the wellness tech community often don’t know each other exists, and they’re all pushing their agenda rather than pushing wellness in general.
We must unite around one message: We’re all a critical part of the healthcare delivery system. Period.
No matter what space you’re in—fitness, yoga, nutrition—if it’s evidence-grounded, you’re part of the healthcare delivery system. And that means we’re essential businesses; governments shouldn’t close us, and we shouldn’t be forced out of business.
We must fight for our status as part of the healthcare delivery system, not just for our business survival, but because what we do saves lives. In the US, it’s crazy how the government has categorized fitness and wellness centers during the pandemic. They put us in the same category as bars and restaurants, perceived as recreation and leisure activity.
Another reason wellness hasn’t become part of healthcare is that we haven’t presented wellness as a multi-pronged total program. One market segment, like yoga, can send the message that they’re the answer and you don’t need anything else. We need a combination of so many things: a sound diet, stress-reduction, strength training, healthy sleep—and you can expand that to dozens of modalities for true wellness. Every one of us in the wellness community needs to help others in the community and send a unified “integrated wellness” message.
Another reason healthcare hasn’t embraced healthy lifestyle choices is that the benefits—especially for mental health—have remained too anecdotal. We must fund and promote evidence-based research on the benefits of holistic approaches to wellness that the medical industry will accept.
The good news is that powerful forces are coming together—from the lessons of the pandemic to young people—that will finally drive wellness to be far more integral to healthcare. Young generations really “get” holistic health and the centrality of mental wellness, and they’re going to shake up the traditional medical/healthcare system.
McGroarty: Your foundation is devoted to changing how the world treats mental health—to think beyond medication and psychoanalysis. How important is the “mental” side in the future of wellness?
Brick: Mental health will be the wellness industry growth driver and will be the mega-force that brings wellness and healthcare together.
I started the John W. Brick Mental Health Foundation with my wife Lynne to honor my brother John, who suffered from schizophrenia his entire life and died from complications caused more by the medication he was taking than the disease. In all his years of treatment, in the best institutions in the world, he was never once put on a well-rounded program that included exercise, nutrition and other healthy behaviors.
life and died from complications caused more by the medication he was taking than the disease. In all his years of treatment, in the best institutions in the world, he was never once put on a well-rounded program that included exercise, nutrition and other healthy behaviors.
We called our foundation a “mental health” —rather than a mental illness—foundation, but we should probably change our name to a “mental wellness foundation.” People are focused on mental wellness like never before, and the stigma of “mental illness” has disappeared almost completely. The main reason that employees now give when they call in sick is depression. Can you imagine telling your boss that 20 years ago?
The future: People seeking all kinds of wellness for the mental benefits. My wife and I have been in the fitness industry for 40 years, and for the first few decades, there were two main reasons people worked out: men to get bigger, women to get smaller. But a recent Euromonitor study found that for every major age group (Gen Z, millennials, Gen X, baby boomers), the #1 reason people now give for working out is for their mental wellbeing.
McGroarty: You’ve spent decades building a bricks-and-mortar fitness empire. Then COVID-19, and it’s all digital, digital, digital. What’s your long-term fitness bet? Digital? In-person?
Brick: In business (as at blackjack tables at casinos), there’s a thing called “table stakes”—the minimum buy-in. In health clubs, it used to be things like good service, clean equipment and aerobics. Today, digital has become table stakes: You have to be online, or you’re toast. But once something becomes table stakes, it’s a commodity, and the price plummets. How many online fitness programs today are free? Hundreds? Thousands? Everything is being done cheaper, faster and better, and if you jump into an online-only fitness business, you need to ponder if it will be financially sustainable two years from now.
Understand what drives your economic engine. As Jim Collins argues in his classic business book, Good to Great, great companies are committed to change while preserving the core. We’re providing online classes both at our high-end, full-service Brick Bodies Space health clubs and at our budget Planet Fitness franchise clubs, but we’re looking at it to complement—not drive—our economic engine, which is health club memberships.
There will always be value in the convenience of doing things at home: working, telemedicine, digital fitness. But it can only go so far because humans are profoundly social beings. Digital will never fully replace face-to-face meetings, work and fitness. The two most important things for mental wellness are coping skills and connectivity. While virtual can give you coping skills, it can never fully replace the connectivity of a live, in-person experience.
That’s why I’m skeptical of the “new normal” and “pivot” concepts. Taking a dramatically different direction that defies human nature is not necessarily the right thing to do. Life will never be the same, but it never is. People will continue to embrace online programs, but they will want their lives back. Their hunger to reconnect will be powerful, and that’s the big, long-term opportunity in wellness.
Digital may be the new “table stakes” in fitness, but the future is still, for the most part, face-to-face community.

McGroarty: The wellness industry has focused on elites, while you’ve been in the budget fitness space for decades. There has been a cry for more inclusivity in wellness. Will this happen? Or is it just virtue signaling?
Brick: In the US, the wake-up to social injustice is as powerful a force as the pandemic. Everyone in wellness needs to make their offerings more accessible, affordable and inclusive because it’s the right thing to do.
But beyond the ethical imperative, the “other 80%” is where the huge market opportunities now lie.
Supply-and-demand is changing fast. Let’s be frank: Twenty years ago, there was almost no demand for wellness programs in minority communities—or for a budget fitness model—because the average person didn’t want to work out.
But I got into Planet Fitness because the affordable fitness space was an untapped opportunity. People always look at markets as pizza pies: There are only so many slices to go around. The “pie” for the health club industry used to be 15–18%, and the industry lived by these laws: never lower your rates, it cheapens the product; raise rates every year; and charge whatever the market will bear. Then Planet Fitness came along and blew that away: Let’s go with $10 a month and just cut out some extras. We have 15 million members today. Do the math: There are 300 million Americans; our members represent 5% of the population. We’ve taken the fitness industry from 18% to 23% of the population. Wow.
But that still leaves an almost 80% opportunity in the US and 90% in other countries. Almost every wellness sector now has the opportunity to dramatically increase its market penetration well beyond that old “15%,” as the demand for wellness is suddenly throughout the general public. A big part of bringing them in will be employers realizing our value and governments supporting our programs as part of healthcare.
Not every wellness business committed to inclusivity needs to think about “the millions.” For some companies, the “top 3%” will always be their core business: A luxury resort can’t just give away 20% of its rooms. But they can do great, inclusive things their way, whether community or online programs. I’m excited because the wellness pie has never been bigger, and there’s an incredible opportunity to expand that pie for everyone, forever.
McGroarty: Name one thing that becomes far more crucial in wellness in the future.
Brick: This crisis drives home the importance of physical and mental resilience.
Over time, because of modern conveniences, humans have devolved. We used to be able to survive in temperatures ranging from 110 degrees to 20 degrees below. Now, any colder than 68 degrees, we heat it; any hotter than 74 degrees, we air-condition it. Because we’ve made our lives so easy and rely on things like medications, we’ve compromised our immune systems and resilience.
We need to introduce more positive stress into our lives to get our bodies to respond and function at peak efficiency.
Positive stress is stress that gets us out of our comfort zone without going beyond what the body can handle: whether running or walking faster, eating less, holding that yoga stretch a little longer, or lifting a little more weight. Our bodies (and minds) respond to positive stress by becoming stronger and more resilient.
The pandemic essentially changes the “why” of wellness—why you push the physical and mental envelope—because we realize now that it’s a matter of survival for all of us.
That’s why our foundation has funded a $1.2 million, gold-standard study with the University of California, San Francisco on how different forms of positive stress—the Wim Hof Method, High-Intensity Interval Training (HIIT), and meditation—impact depressive symptoms. Results are coming soon.
Resilience will be the new cornerstone of wellness, and the industry needs to come together on this message.
We want to hear from you
Why has healthcare resisted integrating preventative wellness approaches for so long? And is the “mental” side the future of wellness?
The post Q&A with Victor Brick: Why the Wellness Pie Has Never Been Bigger appeared first on Global Wellness Institute.
]]>The post Q&A with Melisse Gelula: Shaking Up The Concept of Wellness: COVID-19, Inequality & More appeared first on Global Wellness Institute.
]]>

In this edition of the Wellness Q&A Series Beth McGroarty, VP, Research & Forecasting, Global Wellness Institute asks:
Has COVID-19 fundamentally changed people’s concept of “wellness”?
What wellness markets will grow fastest in the future?
What do the successful wellness brands of the future look like?
Will the new conversations around racial inequality in wellness impact the industry long term?
Q&A with Melisse Gelula, co-founder of Well+Good, a pioneering digital media company

Melisse Gelula was named one of 9 Most Creative Entrepreneurs by Inc magazine and one of 10 Writers and Editors Who Are Changing the National Conversation by Adweek. She has shared her expertise with Good Morning America, CBS This Morning, the New York Times, WSJ, Fast Company, and more. Having grown her company to a successful acquisition, Melisse now advises mission-driven wellness brands in tech, beauty and more. Previously, she worked in mental health as a psychoanalytic therapist and crisis counselor. She is a Global Wellness Institute Board Advisor and recently contributed to the organization’s white paper Mental Resilience in a Time of Stress and Trauma. Currently, Melisse is researching midlife psychosis and motherhood for her forthcoming book, a memoir about being raised by a mother who lived with untreated schizophrenia.
VP, Research & Forecasting, GWI, Beth McGroarty: Has COVID-19 shaken up people’s concept of wellness? If so, how?
Melisse Gelula: Pre-COVID, wellness was increasingly associated with very consumer-y trends—the $17 organic salads, $60 collagen supplements, and the $150 leggings. It was increasingly seen as being a very elitist and privileged industry. But when the pandemic hit, all of us, everywhere, suddenly found ourselves facing something huge and serious: We desperately needed things in our everyday lives to help fortify our health, our sanity, our communities, and our homes. Overnight, people woke up to the importance of more real, accessible wellness for themselves and their families. And this crisis has been a wellness wake-up call for people who may not have been open to it before.
“Pre-COVID, wellness was increasingly associated with very elitist, consumer-y trends—the $17 organic salads, the $150 leggings. With the pandemic, wellness instantly became more vital in a Maslow’s hierarchy of needs kind of way. The word “wellness” will lose some of its stigma.”
Many of us have been arguing forever that wellness is a lifestyle; many of us have been fighting for the idea that wellness needs to be more accessible to all. This crisis has provided proof for that in ways that everyone can understand. Wellness has become more vital in a Maslow’s hierarchy of needs kind of way. So, I see the word “wellness” losing some of its stigma. And if health and wellness once occupied separate channels, now I see them—happily—coming closer together.
During the pandemic, we’ve seen people rushing to proven, beneficial wellness practices that cost little or nothing: learning or practicing meditation or getting out in nature and walking. There’s much data that shows the ways that people worldwide are restructuring their lives around wellbeing practices. For instance, Pinterest released amazing data around their search terms in the middle of the pandemic (February to May 2020), and they saw record searches around mental wellness concepts, with meditation up 44%, gratitude up 60%, and positivity up 42%. Searches around bringing wellness into the home, stress relief, and exercise all saw huge gains. A host of self-care and wellbeing practices suddenly became the coping strategy for more people in the new normal.
GWI: You’re now advising a number of wellness start-ups and are deep in how investment and the market are changing. What categories in wellness do you see growing fastest and mattering most in the future?
“Solving for mental health and wellness will be the biggest future opportunity in the industry.”
Gelula: Yes, I’ve started advising mostly female-founded, first-time entrepreneurs in the wellness space, and most are digital brands that have come up during the pandemic to solve real problems—and our world has a lot of them. This is very interesting to me because building and marketing another kombucha or protein bar brand is not a real problem to solve.

Solving for mental health and wellness will be the biggest future need and opportunity. A recent study by JAMA found that depression rates have tripled for Americans during the pandemic. And yet, mental health is simply the most bewildering, overlooked area in healthcare (and I was a psychoanalyst-in-training and saw people in deep crisis for many years): It’s hard for even really high-functioning people to find a therapist or figure out how to pay for one. It’s funny, all the wellness from “our neck up”—much of our therapy, our mindfulness, even our eye care—is largely privatized and out-of-pocket. It’s been so difficult, but with a massive mental wellness crisis underway, this can no longer be a luxury; it needs to be an essential service.
There’s so much innovation going on in teletherapy and with digital mental wellness platforms, with more funding flowing into this space in 2020 than for any wellness sector. Digital is going to be a far more affordable and democratizing play for the mental health and inner life space, and we will see many revolutionary ideas coming to our devices that shake up how mental health services get delivered. Many of the great ideas will come from outside the traditional mental health industry, and entrepreneurs and practitioners will come into the market without ever having had a brick and mortar business. Some of the newly emerging companies I’m working with are creating more relevant mental wellness platforms for Gen Z and the younger generations. We will also see companies many of us are familiar with coming out with new products that make mental health/wellness more accessible in the next six months.
It’s interesting and telling that even social media platforms, spurred by the pandemic, are now grabbing the mental wellness wheel. There have been a bunch of synergistic partnerships: Snapchat has launched new tools and content around mental wellness and has partnered with Headspace to deliver meditation and mindfulness. Pinterest has created emotional health resources, pins and content, partnering with the Stanford Lab for Mental Health Innovation. These mental wellness moves from social media companies are helping them reach the loneliest, most depressed and anxious generation: the young.
There is so much to say, to rethink, and to invent around mental health and wellness. This is why I’m now writing a book on the topic (framed as a memoir), as I had a mother with schizoaffective disorder who experienced hallucinations and severe mental health challenges. It’s something I’ve never talked about publicly, but this is the conversation our world needs most now and the most important space in wellness.
“A sea change is coming to corporate leadership and career and workplace wellness.”
Another area that will go through a sea change is corporate leadership and career and workplace wellness. We were already facing an employee burnout and mental wellness crisis pre-pandemic. And now employees are radically more overwhelmed: financially, fearing for their safety, and with people thrust into working from home, they’re crushed by juggling family and their jobs, with a fast-dissolving boundary between life and work. It’s so bizarre: It’s as if we’re returning to a time before the Industrial Revolution when all commerce came out of people’s homes and property, but now it’s digital work with an always-on mindset. I’m hearing scary stories: Companies saying, well now that you don’t have commute time, we will start work and meetings at 7:30 AM.
This is impacting everyone, it’s infuriating, and companies (not just employees) are going to have to set real boundaries. For ages, companies drew a hard line (9 to 5) when it came to their role in employees’ lives, and they wouldn’t get into or support, say, their mental health issues because that’s “too personal.” We’ve had to drag companies into offering things like paid leave and mental health days. But companies never seem to mind if their work keeps encroaching further and further into all hours of our lives.
The pandemic is accelerating how frustrated people are with how work is taking over our lives and with the lack of opportunity in the job market (and this is especially true of millennials). I think we will go through a corporate culture and conscious leadership revolution, and it will become crystal-clear who’s caring for their employees and who’s not. More companies will adopt a really human-focused and solutions-oriented mindset, with the rise in a more conscious, empathetic style of leadership that not only helps people feel safe but motivated, supported and actually cared for. If we don’t have this leadership sea change now, it will cripple the workforce. A lot of conscious leadership programs, tools and apps are now coming to the fore. (I just did a program created at Google that focuses on emotional intelligence.) And new approaches to workplace wellness and corporate leadership will be very important for all industries and an opportunity for the wellness market.

GWI: The Black Lives Matter movement has shined a more pitiless spotlight on racial inequities in access to both healthcare and wellness, exposing how white and elitist the wellness market can be. Do you think these new conversations will impact the wellness industry in the long term?
Gelula: First, it’s fantastic to see so many wellness brands by people of color finally getting recognition. But I feel that there has been a lot of pretending in the wider wellness space that equality has been addressed and that they don’t really need to be part of any solution. Every company needs to be part of a solution and seek real equality because wellness is now increasingly political, whether you want it to be or not. Every wellness company needs to make sure that the experiences and brands they create are highly inclusive, whether for people of color, aging people, or LGBTQ consumers. They have to ask themselves the hard questions about the mix of their executive teams and have honest conversations with people of diverse populations on their teams about how they could make their offerings and their company more authentically inclusive.
“It’s not acceptable to NOT take a stance on diversity now. Diverse wellness brands will now grab the limelight, and those seen as failing on this will increasingly receive blowback. There’s a lot of un-following going on.”
It’s not acceptable to NOT take a stance on diversity now. I predict diverse brands will now also grab the limelight, and those seen as failing on this will increasingly receive blowback. People—especially young generations—are savvy and get turned off by tone deafness or lack of real acknowledgment of Black Lives Matter by companies; there’s a lot of un-following going on.
It’s all part of the great transitional moment we are in right now, and so many positive things could come from it. I think we will see it from an eagle-eye perspective in a few years: More companies will have moved from a narrow profit-focused model to a human-focused model in business. Companies that can roll with that will be the ones consumers believe in and buy from and that employees commit to. Eric Weisberg recently argued in Fast Company that the experience of the pandemic means that every brand now needs to behave like a health or wellness brand. This includes wellness brands not walking the talk. It means showing empathy and really relating to the needs and pain-points of your customers (and your employees, I’d add)—and right now, that means respecting their wallets, given the devastating economic situation. Tom’s donated a pair of shoes with each shoe purchase for years. We’re going to see more giveback and pay it forward models like this.

GWI: Any last thoughts on any big picture changes you see coming to the wellness market?
Gelula: The brands that solve real problems will succeed, and we have a whole lot more big problems to solve. Companies that just “sell stuff” and the things that people used to gravitate toward on Instagram (peddled by all those lifestyle influencers) are fading fast. Wellness is no longer a nice to have; it’s a need to have for people, and wellness brands have a huge opportunity to show up and tackle actual needs. We will see more companies and products that are really essential services—whether in mental wellness, in work solutions, in healthy food. The future of the wellness market is a new kind of problem-solving: More solutions-minded wellness businesses that can reach far more people.
It’s a “get real” moment, and all of a sudden, there is more discussion, innovation and investment in what were once stigmatized categories. For instance, in the healthcare tech space, I’m working with a brand called Poppy Seed Health that is solving for unmet maternal health needs (and the high maternal death rate in the US, especially for women of color) by connecting women 24/7 via text to nurses, midwives and doulas, and which also has a miscarriage community for women to talk about this painful topic openly. In beauty, I’m working with a company that is designing products for Indian women and their complexion concerns, a market that has never been addressed.
There are so many gaps in our healthcare system, in our mental health system, in the work/career space, even in beauty that wellness is seeking to fill, and digital companies can play a huge role. But digital companies or not, this is a massive opportunity for wellness to really step up—and act more responsibly—as an industry. And that’s truly exciting.
We want to hear from you
Do you think COVID-19 is changing people’s concept of wellness? And will conversations about racial inequality in wellness impact the industry long term?
The post Q&A with Melisse Gelula: Shaking Up The Concept of Wellness: COVID-19, Inequality & More appeared first on Global Wellness Institute.
]]>The post Q&A: Dr. Nicola Finley Tackles the Deep Inequities in Access to Wellness for Black and Brown Communities appeared first on Global Wellness Institute.
]]>

In this edition of the Wellness Q&A Series Beth McGroarty, VP, Research & Forecasting, Global Wellness Institute asks:
Why is it so urgent to tackle the deep inequities in access to wellness for Black and brown communities? What are some differences in the wellness concept within the Black community? How are women of color being served by the spa/wellness industry? What is the most undervalued approach in wellness?
Q&A with Nicola Finley, MD, Canyon Ranch, Tucson, Arizona

Dr. Nicola Finley practices integrative medicine at Canyon Ranch in Tucson, which opened last week after being closed since March because of COVID-19. She has a passion for women’s health and preventive medicine. Previously, she worked for over 10 years with Tucson’s economically disadvantaged communities at El Rio Community Health Center and St. Mary’s Hospital—experiences that make her well qualified to address the health inequities in Black and brown communities.
She is a graduate of Brown University, received her medical degree from the George Washington School of Medicine, and is board certified in internal medicine. She completed a fellowship in integrative medicine at the University of Arizona and is an adjunct faculty member at the Mel and Enid Zuckerman College of Public Health at the University of Arizona.
VP, Research & Forecasting, GWI, Beth McGroarty: COVID-19 is exposing the terrible racial inequities in healthcare, with Black Americans and Latinos being hospitalized at four to five times the rate of white people. But what about the profound inequalities in access to wellness? Why must we specifically bridge that gap? What most needs to change?
Dr. Nicola Finley: If you want to tackle the profound racial disparities in health, you have to create better access to wellness and preventative medicine because Black and brown people—as COVID-19 is painfully laying bare—have much higher rates of chronic diseases (heart disease, diabetes, hypertension, obesity and chronic kidney disease), and the wellness concept and industry could help prevent and manage those conditions.
The first thing we need to do is honestly acknowledge that racial disparities in both healthcare and wellness exist. People and businesses may think of themselves as colorblind, but that doesn’t solve the problem because it doesn’t allow you to embrace person-centered care. Traditional medicine is focused on the biology of illness; it’s not focused on the whole person. What COVID-19 exposes is that we should embrace integrative medicine because it addresses the whole person (their body, mind and spirit). The integrative model embraces the idea that a person’s ethnicity, environment, emotions, family structure, and lifestyle (whether access to exercise or healthy food) have a huge impact on their health. In integrative medicine, we try to see the whole person; we listen; we validate them.
For so long, many people of color have not felt seen, heard or valued by the wellness industry. While wellness organizations have been working  on this – they need to become more explicitly inclusive, listen to communities of color, and realize there is great diversity within those communities. People of color may feel unwelcome in the wellness space because it’s so homogenous. I speak for myself as a Black woman: I don’t necessarily need my provider to be a Black provider, and I feel comfortable if I’m the only Black person in the room, but it’s far more welcoming when everyone is not the same race, age, body type and/or socioeconomic background. Observational diversity— in terms of race, gender, body type, age or disabilities —really helps. I do see positive industry evolution: new wellness solutions being designed specifically for African-Americans, for Latinas, for the LGBTQ population—where they get their own spaces and lane. There is much more work to be done. And we have to look inward to overcome the inequities in wellness and to do what we can to welcome people of color.
on this – they need to become more explicitly inclusive, listen to communities of color, and realize there is great diversity within those communities. People of color may feel unwelcome in the wellness space because it’s so homogenous. I speak for myself as a Black woman: I don’t necessarily need my provider to be a Black provider, and I feel comfortable if I’m the only Black person in the room, but it’s far more welcoming when everyone is not the same race, age, body type and/or socioeconomic background. Observational diversity— in terms of race, gender, body type, age or disabilities —really helps. I do see positive industry evolution: new wellness solutions being designed specifically for African-Americans, for Latinas, for the LGBTQ population—where they get their own spaces and lane. There is much more work to be done. And we have to look inward to overcome the inequities in wellness and to do what we can to welcome people of color.
I have worked with underserved populations: I spent 13 years at El Rio community health clinic in Tucson, where I had the privilege of taking care of mostly Mexican-American and Native-American (the Pascua Yaqui tribe) patients. And with respect, what I learned firsthand was the lack of access to quality healthcare and the low health literacy rates among these populations. If the wellness industry wants to help bridge the health/wellness gap, they could really help with health literacy and prevention for underserved populations.
I graduated from medical school in the 90s, where there was a movement for doctors to achieve “cultural competency;” that’s where you learn about a person’s culture so you can be competent to take care of them. While cultural competency is so important, we now know that’s not enough: We should also be trained in and practice cultural humility. That means (whether you’re a doctor or a wellness practitioner) that you not only learn about other cultures but you also practice self-reflection and self-critique about your own implicit biases and how that impacts your care. It means being humble, and humility can be uncomfortable and takes courage. Working on cultural humility is crucial in the wellness space because there’s just not enough diversity among providers yet. For instance, dieticians and nutritionists are overwhelmingly not from communities of color. But practitioners can take better care of diverse and vulnerable populations if they practice cultural humility in addition to cultural competency.
GWI: “Wellness” means different things for different populations. What are some differences in the concept for the Black community?
Finley: First, it’s important for the wellness industry to ask communities of color how they define and practice wellness. It may look pretty different than how the media portrays wellness. In many Black communities, the concept often has spirituality at the center, which gives a person a sense of purpose and a real community of connections (all of which powerfully impact health). Many want their doctor to acknowledge and talk to them about their spirituality—however they define it. In general, I’ve also found that Black and brown communities embrace a more integrative concept of health, not just traditional medicine but also a great openness to natural and alternative approaches.
Speaking specifically about Black and brown women and how we’re raised, we’re raised to be caregivers of our family and to nurture others. This is case for me, with my immediate and extended family. My parents are immigrants from Jamaica, and Jamaica’s motto is “out of many one people.” It’s all about embracing multiculturalism and taking care of others. But the problem is that we oftendon’t take care of ourselves. I think more people of color would explore the wellness space if people didn’t say, “Oh, you’re getting another massage…you’re taking another vacation,” because the message within communities of color should be, I’m so happy that you’re seeing the importance of taking care of yourself with self-care practices.
GWI: The representation that the wellness industry is intensely white doesn’t reflect what I hear when I talk to wellness businesses and spas, where women of color are a passionate customer base. They’re THERE, but how do you think they are being served?
Finley: We’ve known for years that Black and Latina women spend more on beauty than white women, but I don’t think the spa and wellness industry has really embraced that. When I go to a spa (and it’s not as much as I would like!), I have to bring my own shampoo and conditioner because whatever they have usually isn’t moisturizing enough for my hair. When I go to a spa that offers makeovers, the makeup colors often don’t work for my skin tone. It’s hard to understand: They want me as a customer, but yet they’re not showing me that. These are little things, but little things add up to something big. If companies want to tap and serve that lucrative market, we need to have people of color in leadership roles that are in a position to make changes and decisions.
GWI: Beyond a more inclusive industry, what is one approach that you think is the most undervalued in the wellness world?
Finley: Dance! I’ve been dancing since I was young – I love to dance, and now I’m a Zumba instructor. My passion for dance increased when  my sister and I started going on the Zumba cruises (which we’ve done every year for the last 5 years). It’s the best time: You’re connected with 3,000 of your Zumba besties, and it’s so international, with someone from India leading a Bollywood-style dance or an African leading an African dance. You get to be yourself: When I dance, I’m not Dr. Finley. I’m just Nicola. It’s just me, the movement, and the music. And now I’m dancing virtually at Zumba.com.
my sister and I started going on the Zumba cruises (which we’ve done every year for the last 5 years). It’s the best time: You’re connected with 3,000 of your Zumba besties, and it’s so international, with someone from India leading a Bollywood-style dance or an African leading an African dance. You get to be yourself: When I dance, I’m not Dr. Finley. I’m just Nicola. It’s just me, the movement, and the music. And now I’m dancing virtually at Zumba.com.
I think dance should be more central in the wellness world because it’s far more than exercise: It’s mental exercise and the most natural way to connect mind and body, which reduces stress. Dance has so many proven benefits: It helps people with Parkinson’s, diabetes, dementia, PTSD, depression and anxiety. It’s amazing for older people because it enhances their cognition and memory, and the quick movements and strengthening of muscle tone really help to prevent falls.
At Canyon Ranch, I partnered with a dance instructor to interweave my lectures about why dance is such powerful medicine with dance sessions. Guests love the fact that their doctor is dancing with them, and it’s such a great way to connect. My favorite week at Canyon Ranch is Gotta Dance Week (three times a year), where we bring in choreographers from across the country (in ballet, tap, Latin influence, hip hop, jazz, etc.). I plan my work schedule so I can attend as many classes as possible. I’ve gotten to know many of the regular dance week guests, and they’ve gotten to know each other. It’s a real community, and it’s exactly what I love about dance: the connection and how everyone feels welcome.
GWI: How do you think COVID-19 will change the wellness market?

Finley: For so many reasons, I think wellness becomes more central to people’s lives and a stronger market. One reason: With so many people working at home (and who knows for how long), some are not turning work off, which could lead to more stress. People may need to reinvent new approaches to achieve work-life balance and self-care is going to be needed so much more.
For everyone, all over the world, COVID-19 just keeps hitting us with so much anxiety: You’re sheltering in place, then you’re not, and then repeat. People are understandably struggling. The wellness world specializes in approaches for anxiety, sleep and mental wellbeing.
Some segments of the population are experiencing an extraordinary crisis. I have many friends who are physicians on the front line, and they’re emotionally and physically exhausted because of this unprecedented pandemic. Physicians who didn’t have difficulty managing stress or anxiety before COVID-19 are now experiencing profound burnout. For example, COVID-19 is brutal for doctors and nurses because striving for excellence and saving lives is in our DNA. With the Coronavirus we’re unable to be as effective as we are with other illnesses, and it’s so unpredictable. Patients are doing well in the hospital, and then their health declines unexpectedly, and healthcare workers are dealing with so much grief and loss. And female physicians are 1.6 times more likely to experience burnout.
COVID-19 may be unleashing so much uncertainty, but the need for “more wellness” in our future seems quite certain.
We want to hear from you
Do you think it is urgent to tackle the deep inequities in access to wellness for Black and brown communities? Are women of color being served by the spa/wellness industry?
The post Q&A: Dr. Nicola Finley Tackles the Deep Inequities in Access to Wellness for Black and Brown Communities appeared first on Global Wellness Institute.
]]>