The post Can Exercise Change the Odds for Cancer? appeared first on Global Wellness Institute.
]]>
October 8, 2025
The post Can Exercise Change the Odds for Cancer? appeared first on Global Wellness Institute.
]]>The post Integrative Oncology and Cancer Self-Help Webinar appeared first on Global Wellness Institute.
]]>
WATCH RECORDING
Integrative Oncology and Cancer Self-Help Webinar
A thoughtful discussion inspired by the Netflix series Apple Cider Vinegar
Wednesday, March 19, 10-11am ET
The recent Netflix series Apple Cider Vinegar has sparked meaningful conversations about cancer, wellness, and the complexities of treatment. The series highlighted many aspects of the cancer journey and raised critical questions about supportive care—the role of integrative approaches in improving quality of life, managing side effects, and empowering individuals to take an active role in their health and wellness journey.
The Global Wellness Institute’s Wellness for Cancer Initiative invites you to a thoughtful discussion on Integrative Oncology and Cancer Self-Help—bridging the gap between conventional medicine and holistic healing.
Join Wellness for Cancer Initiative Chair Julie Bach, cancer health coach with the Society for Integrative Oncology (SIO) and SIO’s Patient Advocate SIG, alongside:
- Lainie Francis, MD, integrative oncologist at Hillman Cancer Center
- Aga Kehinde, cancer nurse and co-chair of the British Society for Integrative Oncology
- Rosy Daniel, MD, integrative medicine physician, former medical director of the Bristol Cancer Help Centre (now named Penny Brohn UK)
- Jean Di Carlo, the Chair of the SIO Patient Advocate SIG





Together, we will reflect on what we saw in the series, listen to what you took away, and explore the evolving role of integrative oncology. This discussion will highlight how integrative approaches such as nutrition, stress management, movement, and mind-body therapies support patients from diagnosis and survivorship.
The post Integrative Oncology and Cancer Self-Help Webinar appeared first on Global Wellness Institute.
]]>The post Wellness for Cancer Initiative Trends for 2024 appeared first on Global Wellness Institute.
]]>2024 Trends
![]()
With the probability of a cancer diagnosis approaching one in two individuals, it becomes critically important to advocate for sustainable lifestyle choices that aim to diminish cancer risk before diagnosis, enhance the effectiveness of cancer treatments and decrease the likelihood of recurrence. The paradigm of cancer management is evolving towards earlier detection and enhanced treatment modalities—with a key pillar of preemptive action through prevention. The insights and trends provided by the Wellness for Cancer Initiative shed light on future directions concerning lifestyle adjustments and highlight the breakthroughs in the domain of cancer precision medicine.
TREND 1:
With Wellness Centers Focused on Longevity, the Impact of Cancer and Its Treatments Need to be a Consideration
Longevity is a big topic in the wellness industry. Many health and wellness centers offer advanced testing, imaging and daily monitoring of vitals to determine areas that can be improved. Research has shown that “the effects of cancer and its treatment are associated with the late occurrence of additional comorbidities that happen earlier or more frequently in cancer survivors compared to cancer-free individuals.”1 This is often known as accelerated aging. Cancer treatments, for example, can affect many vitals, such as heart rate variability. If the health practitioner is focused on longevity, it is important that they interpret the client’s data and gain an understanding of the client’s full health history–and place it in proper context–before measuring them against general population numbers. While the lifestyle intervention may be the same or similar to non-cancer-affected individuals, the root cause of the health measurement is not necessarily the same. Current research is exploring the effectiveness of proactive lifestyle strategies and pharmacological interventions to slow down or potentially reverse the aging process. Lifestyle strategies include prehabilitation, dietary adjustments like caloric restriction and rehabilitation programs. According to PubMed, the use of senolytics (a class of drugs that selectively clear senescent cells, which are said to accumulate with ageing) includes both pharmacological and natural occurring (e.g., quercetin). Ultimately, these interventions are aimed to address health span and lifespan. Further research will be of paramount importance as the number of cancer survivors continues to grow.
Sources:
- Bhatia R, Holtan S, Jurdi NE, Prizment A, Blaes A. Do Cancer and Cancer Treatments Accelerate Aging? Curr Oncol Rep. 2022 Nov;24(11):1401-1412. doi: 10.1007/s11912-022-01311-2. Epub 2022 Jul 7. PMID: 35796942; PMCID: PMC9606015.
TREND 2:
Wellness Centers Focus on Longevity: Some Are Considering Early Cancer Detection Tests
The medical industry has made remarkable advancements in the treatment of cancers, including precision medicine (targeted therapies) and CAR T cell therapies. The field of oncology is also witnessing a remarkable transformation with the introduction of cancer early detection tests, including the promising multi-cancer early detection (MCED) tests. Several wellness centers and wellness conferences have discussed the role of early cancer detection tests. Our trends two years ago pointed to the promising GALLERI test as an example. This year’s trend is an addendum to that trend.
The Emerging Landscape of Early Cancer Detection Tests
The field of oncology is witnessing a transformation with the introduction of cancer early detection tests, including the promising MCED tests. These advancements aim to overhaul traditional cancer screening methods by providing a broader, more efficient and potentially more effective approach to identifying cancer early through the detection of circulating tumor DNA from a wide variety of cancers in a non- or minimally invasive manner.
What are MCED?
Multi-Cancer Early Detection tests are groundbreaking in the realm of oncology, capable of detecting multiple types of cancers before symptoms manifest. Utilizing cutting-edge technologies, such as next-generation sequencing and liquid biopsies, MCED tests analyze samples for molecular signs of cancer, offering a new frontier in early diagnosis and significantly boosting early diagnosis rates across multiple types of cancer.
The Benefits
MCED tests herald a considerable promise for enhancing cancer survival rates via early detection, providing the opportunity for treatments to start sooner when the cancer is more manageable. By screening for various cancers through a single test, MCEDs can simplify the detection process, potentially streamline healthcare workflows, and offer a more cost-effective solution than conventional screening methods targeting one cancer at a time.
The Harms
Despite their potential, MCEDs come with their share of concerns, including the risks of yielding false positives that can lead to unnecessary stress, anxiety and invasive follow-up procedures for individuals. Additionally, the possibility of false negatives may delay essential treatment. Concerns also extend to the risk of overdiagnosis, possibly resulting in the treatment of cancers that may not pose a significant threat to health and the potential to exacerbate healthcare inequalities.
Wellness Centers Must Consider
For wellness centers and spas considering the inclusion of MCED tests among their offerings, it’s paramount to ensure informed decision-making processes for clients through detailed consultations with genetic counselors and specialist oncologists. An interdisciplinary approach, integrating expert interpretation of test results and establishing a protocol for managing false positives and educating clients about overdiagnosis, can mitigate potential harms and bolster the efficacy and relevance of MCED tests in the health and wellness industry. Collaboration with oncologists is crucial to providing comprehensive, accurate and responsible care, ultimately enhancing the value of cancer screening services in these settings.
Variables to Address If Considering Cancer Screening Tests
- Ensure Informed Decision-Making: Prior to undergoing MCED tests, individuals should engage in comprehensive consultations with genetic counselors and specialist oncologists. This step is crucial to fully understanding the test results’ benefits, limitations and potential implications.
- Integrate Expert Interpretation: To avoid misinterpretation of MCED test results, it’s essential that these tests are interpreted by healthcare professionals with expertise in cancer genetics. Accurate interpretation is key to making informed healthcare decisions.
- Adopt a Holistic Approach: Spas and wellness centers offering MCED tests must actively partner with medical facilities to ensure a holistic approach toward client health. This partnership should facilitate access to medical consultation and counseling, blending wellness with medical vigilance.
- Address False Positives Proactively: Institutions offering MCED tests should establish protocols for managing false positives, including clear guidelines for follow-up procedures. This reduces unnecessary anxiety and invasive follow-up for clients.
- Educate on Overdiagnosis: Clients should be educated about the phenomenon of overdiagnosis through MCED tests. Understanding that not all detected abnormalities may lead to serious health issues is important for informed decision-making.
Importance of Alliance with Oncologists for Wellness Centers
Wellness centers conducting MCED screenings should prioritize establishing an alliance with oncologists rather than relying solely on the healthcare providers within the resort. This strategic partnership is crucial in ensuring that clients are supported throughout the screening process and provided with accurate and comprehensive information from the outset. Oncologists bring specialized knowledge and experience that are indispensable for interpreting MCED test results accurately and advising on the best course of action. This alliance ensures that clients receive guidance grounded in oncology expertise, facilitating informed decision-making and support through any necessary medical interventions. In essence, by collaborating closely with oncologists, wellness centers can enhance the effectiveness, reliability and overall value of their cancer screening services, positioning client wellbeing and proper care at the forefront of their operations.
Sources:
- Multi-Cancer Early Detection: The New Frontier in Cancer Early Detection, Carmen E. Guerra, Prateek V. Sharma, Brenda S. Castillo, Annual Review of Medicine 2024 75:1, 67-81
TREND 3:
Cancer Health & Wellness Coaching Are Growing in Cancer Care
Health coaching is beginning to emerge as a vital component of integrative medicine, playing a pivotal role in cancer prevention and aiding individuals in navigating the complex landscape of cancer diagnosis, treatment and recovery. It serves to enhance the quality of life and, in certain instances, contribute to improved clinical outcomes for those affected by cancer. A cancer health and wellness coach is a professional dedicated to working with individuals either directly as a client or in conjunction with a healthcare professional or hospital, providing support throughout their cancer journey. These coaches often work in conjunction with a team of medical doctors, dietitians, nutritional therapists, psychologists or counselors. Their role complements that of the traditional healthcare team by focusing on lifestyle factors that bolster overall health, wellness and wellbeing.
The primary objective of cancer health and wellness coaching is to empower individuals to take an active role in their care, making informed decisions that resonate with their unique circumstances and personal preferences. This self-empowering approach is centered around translating and personalizing generic lifestyle advice often provided by health professionals. Cancer health and wellness coaches emphasize the importance of aligning their support with the individual’s wishes, circumstances, preferences, needs, values and cultural background, ensuring a compassionate, dignified and respectful support system.
One of the initial steps in cancer health and wellness coaching involves helping individuals recognize and believe in their daily actions’ influence on their care and outcomes. Coaches work on establishing a personal connection, focusing on the individual as a unique entity seeking to improve their cancer journey through sustainable lifestyle changes across six pillars: physical, emotional, spiritual, social, intellectual and occupational.
Highlighting the efficacy of health coaching, clinical data points to significant benefits such as improved physical activity levels, reduction in cholesterol, levels, better self-management, reduced diabetes risk, decreased hospitalization rates and alleviation in pain severity. Specifically for cancer patients, health coaching offers personalized support that enhances understanding of their condition, builds self-efficacy, encourages the adoption of healthier habits and aids in reframing negative patterns to boost overall wellbeing.
The American College of Lifestyle Medicine’s (ACLM) Compendium of Health and Wellness Coaching and its 2019 Addendum underscore the effectiveness of health coaching as a behavior change methodology. This body of evidence supports the application of health coaching in the prevention and treatment of various conditions, including diabetes, hypertension, heart disease, and, notably, cancer, among other chronic disorders.
Sources:
- Julie Bach, Cancer Health & Wellness Coach, Educator of Cancer Health & Wellness Coaching
- https://www.oncio.org/blog/blog-post-what-is-health-coaching
- https://osarahealth.com/healthcoaches
TREND 4:
National Cancer Institute (NCI) Continues to Fund Exercise and Nutrition Interventions to Improve Cancer Treatment-Related Outcomes
The newest lifestyle and survivorship research is being conducted at Sylvester Comprehensive Cancer Center, which is part of the University of Miami Miller School of Medicine. It aims to explore the effects of nutrition and exercise on cancer therapy and its outcomes. These efforts seek to understand how integrating lifestyle medicine into clinical practice can enhance cancer care.
Spearheaded by Tracy E. Crane, PhD, RDN, who co-leads the Cancer Control Program and directs lifestyle medicine, prevention and digital health at Sylvester, the initiative is poised to revolutionize how patients receive care by incorporating nutrition and exercise support seamlessly into their treatment plans. That being said, other cancer treatment centers across the US and around the world are also pursuing integrated wellness-medical treatment plans.
Dr. Crane and her team are considered at the forefront of leveraging digital health and technology solutions developed within her lab to integrate lifestyle medicine into clinical settings effectively. Their work is instrumental in ensuring that every cancer patient benefits from tailored nutrition and exercise recommendations, which could play a pivotal role in improving therapy outcomes. By using digital technology, the team aims to make lifestyle medicine an integral part of every patient’s cancer care regimen, emphasizing the potential of technology in facilitating this groundbreaking approach.
Sylvester Comprehensive Cancer Center has taken a significant step forward by participating in the Exercise and Nutrition Interventions to Improve Cancer Treatment-related Outcomes (ENICTO) in Cancer Survivors consortium, funded by the National Cancer Institute (NCI). This study is one of the consortium’s four trials and is poised to contribute to and benefit from shared knowledge and practices in enhancing the efficacy of cancer treatments through lifestyle interventions.
Sylvester is also collaborating with Yale researchers on the Trial of Exercise and Lifestyle in Women with Ovarian Cancer. This study seeks to ascertain whether lifestyle interventions can assist patients in completing their chemotherapy regimens, potentially opening new avenues for improving treatment adherence and outcomes. Such collaborative efforts underline the critical importance of lifestyle factors in complementing traditional cancer treatments.
Additionally, Dr. Crane and colleagues are deeply involved in the Lifestyle Intervention of Food and Exercise for Lymphoma Survivors (LIFE-L) trial. This trial examines whether adopting the Mediterranean diet and engaging in regular exercise could enhance chemotherapy completion rates among lymphoma patients.
These initiatives underscore a holistic approach to cancer care, emphasizing the synergistic role of nutrition and exercise in supporting cancer therapy and potentially improving the lives of those affected by cancer.
Sources:
TREND 5:
Studies Examine Feasibility and Clinical Utility of Utilizing Handheld Devices to Detect Breast Cancer
Breast cancer, the most common cancer globally, exhibits a stark contrast in detection and survival rates between high-income countries (HICs) and lower- and middle-income countries (LMICs). While HICs often detect breast cancer early, leading to survival rates of 80%-90%, LMICs face late detection due to inadequate clinical evaluation and screening infrastructures, resulting in a 40%-60% survival rate. This disparity emphasizes the urgent need for accessible screening methods in LMICs, where more than half of global breast cancer incidences occur.
To address this gap, the Intelligent Breast Exam (iBE) device was developed and approved by the US Food and Drug Administration in 2013. This innovative, handheld device offers a cost-effective, portable solution for breast examinations without the need for radiation, relying instead on sensors to electronically palpate the breast tissue and identify abnormal tissue elasticity indicative of potential malignancies. The device’s piezoelectric finger (PEF) measures tissue compression, highlighting differences in tissue elasticity which could point to the presence of a lesion. It presents findings in a straightforward manner, using color-coded 3D maps to distinguish between normal tissue and suspicious areas without necessarily necessitating professional interpretation.
Further enhancements in its technology led to the second-generation iBE system, which includes a Dynamic Co-Planar Capacitive Sensor (DCPC Sensor) and a mobile application, iBreastExam Connect, that facilitates the documentation and sharing of up to 10,000 breast examinations for efficient comparison of results over time.
In LMICs, the limited access to healthcare facilities, shortage of trained providers and prevalent cultural and psychosocial barriers significantly contribute to the late detection and higher mortality rates associated with breast cancer. The iBE device emerges as a promising tool for early screening and triaging, potentially mitigating these challenges by enabling early detection without the need for expensive, conventional diagnostic imaging. This innovative approach could be pivotal in reducing the global health disparities in breast cancer mortality and incidence, particularly benefiting LMICs with resource-limited settings.
Sources:
- ”Can the Clinical Utility of iBreastExam, a Novel Device, Aid in Optimizing Breast Cancer Diagnosis? A Systematic Review. JCO Global Oncolology, 2023 by American Society of Clinical Oncology. https://ascopubs.org/doi/10.1200/GO.23.00149
TREND 6:
Early Diagnostic Testing for Ovarian Cancer Using AI and Imaging Enhancements
AI-Powered Early Diagnostic Test
Researchers are developing an early diagnostic test for ovarian cancer through the application of AI technology. This innovation aims to address the challenges of early detection, as currently, only 20% of ovarian cancers are diagnosed early. The lack of early symptoms and effective screening tests similar to those for breast and cervical cancers contributes to late diagnoses, often when the disease has advanced to critical intra-abdominal organs.
FDA-Approved “Glowing Tumor” Imaging Drug
The FDA has approved a novel imaging drug, known as Cytalux, which makes ovarian cancer cells “glow” during surgery, improving the accuracy of tumor identification and removal. This breakthrough, pioneered by surgeons at the University of Pennsylvania, along with their extensive research in targeted imaging technologies for various cancers, significantly enhances surgical precision. By illuminating tumors, surgeons can identify and resect cancerous lesions that would otherwise be missed, improving patient outcomes. This approach has been tested in a multi-center Phase 3 study, showing promising results in detecting cancerous lesions not found through traditional methods.
Sources:
- https://research.gatech.edu/researchers-leverage-ai-develop-early-diagnostic-test-ovarian-cancer
- www.pennmedicine.org/news/news-releases/2021/november/fda-approves-glowing-tumor-imaging-drug-to-better-identify-ovarian-cancer-cells
The post Wellness for Cancer Initiative Trends for 2024 appeared first on Global Wellness Institute.
]]>The post Wellness for Cancer Initiative Partners with Anticancer Lifestyle Program appeared first on Global Wellness Institute.
]]>
Wellness for Cancer Initiative Partners with Anticancer Lifestyle Program making resources available worldwide to the wellness and cancer community.
Your Lifestyle Matters.
he Global Wellness Institute (GWI) Wellness for Cancer Initiative led by Chair Julie Bach and Vice Chair Shamali Singhal, MD, was formed to bridge the world of wellness with the world of medical. The Initiative has partnered with the Anticancer Lifestyle Program to provide awareness, resources and a call to action for the wellness industry and cancer community that recognize “Your Lifestyle Matters.”
Watch this a minute-long video on the Anticancer Lifestyle Program here. Share it with people you know interested in reducing their risk of cancer or to support someone you know with cancer.
This partnership follows up on the 2022 GWI Wellness for Cancer Initiative Trend, The Only Way Forward is Prevention, and the 2023 trend, Your Lifestyle Matters in all stages of life and phases of cancer from prevention onward. Through this partnership, the organizations will:
- Share high quality educational content, interactive videos, recipes and content from leading global Integrative Oncology researchers and experts on anticancer lifestyle options.
- Increase awareness on anticancer lifestyle choices for prevention of cancer, management of side effects and enhanced quality of life through treatment, as well as in cancer survivorship or end of life.
- Provide resources to the global community to shape the conversation on cancer awareness through all phases of life.
Learn more about their initiative the GWI Wellness for Cancer Initiative, and the Anticancer Lifestyle Program.

The Anticancer Lifestyle Program provides the resources you need to make healthy and informed lifestyle choices that can reduce your risk of cancer, cancer recurrence, and chronic illness.
The post Wellness for Cancer Initiative Partners with Anticancer Lifestyle Program appeared first on Global Wellness Institute.
]]>The post Wellness for Cancer Initiative Trends for 2019 appeared first on Global Wellness Institute.
]]>2019 Trends
Building upon the progress made the past three years, The Wellness For Cancer Global Wellness Institute Initiative predicts that wellness will continue to become more accessible and tailored to all guests, including individuals at risk of or touched by cancer. Leading this integrative lens are wellness hotel and destination brands and preeminent skin-care brands that are integrating cancer awareness as a strategic customer service initiative that is embedded within their overall business and operational strategies, including customer touch points (e.g., spa and wellness service and programs, food and beverage), product/service development, and community outreach.
TREND 1: Spa and Wellness Industry becomes serious about being Cancer Aware by establishing minimum education standards
As the spa and wellness industry continues to have more open conversations about being cancer aware, global training standards will emerge as currently the entry level of therapist training varies significantly. Cancer treatments affect all systems of the body, and the ability to tailor a massage or beauty treatment rest on the foundational knowledge of a therapist and not on a one set protocol that purports to be appropriate for every body.
TREND 2: Beauty not only moves to being clean but also into being Cancer Aware
With shifting statistics of 1 in 2 individuals being diagnosed with cancer during their lifetime and the consumer push toward being clean to avoid cancer-causing ingredients, skin-care brands recognize the need to study and communicate which of their products can safely be used by clients whose skin has been impacted by cancer treatments and whose skin health is comprised of various skin types all at the same time.
While testing of skin-care ingredients and the impact on people in cancer treatment is poor and virtually nonexistent, brands will test their products with clients to ensure to the best they can that clients won’t have skin reactions to their products at a time where there is little tolerance by the client for additional adverse skin reactions.
TREND 3: Wellness Brands apply principles of healthy living to people touched by cancer
Leading wellness brands will adapt principles of breathwork, meditation, focused attention exercises, yoga asana, exercise and plant-based diets to people touched by cancer to support healthy living, resiliency, and the way in which the mind and body functions to express themselves. Additionally, brain health exercises that can be applied to all aging individuals have been shown to improve cognitive function in cancer survivors with respect to attention, brain speed and memory, resulting in less anxiety, depression and fatigue.
TREND 4: Sleep programs will address circadian rhythms from cancer prevention through cancer treatment and into survivorship
While the wellness industry is deploying a spectrum of sleep programs, the importance of circadian rhythms can be extended from cancer prevention, through cancer treatment and into survivorship. With disrupted circadian rhythms linked to cancer biology of several cancers (e.g., breast, prostate and colorectal cancers), insomnia affecting up to 80 percent of individuals with cancer, and sleep disturbances reported to last up to 10 years post cancer treatment, the importance of helping guests explore ways to improve their sleep is vital.
TREND 5: Menopause programs assist women with lifestyle changes for cancer prevention, through cancer treatment and to prevent the risk of recurrence
Newly launched menopause programs help individuals manage symptoms, such as hot flashes, mood disturbances, sleep, skin health and psychological issues associated with the process of menopause.
These programs can also address the nutritional and physical aspects of functional aging, which include the increased risk of breast cancer after menopause. While menopause itself doesn’t increase breast cancer risk, an aging body does.
The culprit—estrogen—with 80 percent of breast cancers in post-menopausal women fueled by estrogen. While certain types of estrogen decrease during menopause, the body continues to produce it in later years with most of it coming from adipose fat cells and adrenal glands. Weight gain during menopause is a risk factor for post-menopausal cancer since more fat cells mean more estrogen. And this type of fat also increases inflammation in the body, which is also linked to a higher risk of breast cancer.
Additionally, menopause programs can be adapted to the many young women who are thrown into medically induced menopause from their cancer treatments.
The post Wellness for Cancer Initiative Trends for 2019 appeared first on Global Wellness Institute.
]]>The post Wellness for Cancer Initiative Trends for 2021 appeared first on Global Wellness Institute.
]]>2021 Trends
TREND 1: The most exciting innovation in early detection–The Galleri test has arrived!
One of the MOST exciting developments in early cancer detection is the Galleri test.
While medical guidelines recommend screening for breast, prostate, colorectal, cervical and lung cancers, over 70% of all cancer deaths are caused by other cancer types that are not commonly screened for.
The Galleri blood test can detect the presence of over 50 different cancers with a 99.5% specificity with one simple blood draw. This means that if the test result is positive for a cancer signal, it has less than a 1% chance that the test is wrong.
- The test is also able to identify the site of the cancer’s origin in the body with an 89% accuracy.
- Of the 12 cancers responsible for two-thirds of all cancer deaths per year in the US, the Galleri test can detect these with a 76% sensitivity.
- The Galleri test is intended to be complementary to and not a replacement for recommended cancer screenings.
It is estimated that if the Galleri test were added to routine cancer screenings, the number of cancers detected in adults in the US through screening could increase from 200,000/year to over 600,000/year, a three-fold increase in cancer detection. Today, many cancers are found too late, leading to poor outcomes,” says Dr. Liu., Mayo Clinic Oncologist “The ability to detect cancer early is critical to successful treatment.
https://newsnetwork.mayoclinic.org/discussion/groundbreaking-early-cancer-detection-test-studied-at-mayo-clinic-introduced-nationally/
https://grail.com/our-products/
TREND 2: Wellness brands evolve to become more inclusive without ostracizing, stereotyping, or collectively grouping individuals by offering the “cancer” service.
Statistics show that 1 in 2 individuals will be diagnosed with cancer. The ability to address and adapt services and programs for individuals requires sensitivity and finesse.
If the medical industry can personalize medical treatments for cancer, surely the wellness industry can adapt any of its services for cancer and many other conditions.
As the wellness industry emphasizes greater personalization, it does not seem sensible or practical to have one menu for healthy clients and another menu for clients with a disease or chronic illness. When we label, we limit thoughts and beliefs about what we think a person is capable of receiving. People diagnosed with cancer are not all the same. What happens when a person has more than one condition? Or with a person living with metastatic (incurable) cancer—does this mean he can only receive “the cancer massage” for the rest of his life?
Individuals living with cancer or touched by cancer are not a demographic. They are just as unique as any other human—each with its own set of wellness preferences. Cancer is only a part of someone’s whole life; it does not define them as a person or their wellness choices. This is an important distinction that the wellness industry is learning and adopting.
During a recent conference hosted by Professional Beauty Group, several cancer thrivers’ voices were shared alongside wellness thought leaders who had experienced or were touched closely by a family member with cancer. Together, they shaped the conversation surrounding their experiences and their hopes for the evolving wellness industry.
- Marina Efraimoglou, owner of Euphoria Retreat and cancer thriver, mentioned that people are “almost” identified by their situation—a breakup, divorce, cancer or chronic situation—but it is our job to help them see that they are so much more than their disease.
- Corrina Yap, director of wellness at Rosewood Hong Kong and cancer thriver, expressed that as an industry, we are still learning, but we cannot “other” individuals (making them separate from) by offering them the disease-oriented service.
- Neil Jacobs, CEO of Six Senses, and John and Karina Stewart, Owners of Kamalaya, each shared personal experiences with cancer and why it is so important to recognize the whole individual by providing the same menu of services for guests and adapting them for each guest’s unique and personal situation.
- Lauri Medina, MD, (oncology surgeon) and Lauren Huffmaster (cancer survivor and executive director of Adventure Therapy Foundation) discussed the need to be more sensitive. A woman aged 30 with two kids is coming in for a service just as any other woman aged 30 with two kids. This woman may even have metastatic cancer, which means she will likely die of cancer, but she cannot allow cancer to define her or her family’s journey. Being normal and living a life that is normal for them is the most empowering way we, as an industry, can be supportive.
- The Bra Sisters (UK) spoke about how women, during cancer treatment and beyond, want lingerie that is more feminine and less medical-looking. They were inspired to start their business based on their personal experience shopping for lingerie and having to go to the back of the store to shop in a sub-set of bras made for people with cancer.
TREND 3: Access to living well and healing evidence and practices from leading doctors and wellness practitioners has never been so readily available.
This past year, while the whole world was experiencing trauma, healing and living well summits surfaced in a variety of ways. Healing as a topic itself applies to everyone, and with the rise in digital summits, there was greater accessibility of quality content from leaders in the fields of healing and wellness.
A multitude of collaborations surfaced—whether cancer-only forums or summits sponsored by cancer organizations and charities OR healing-focused summits with cancer as a common thread.
We provide three inspiring examples where cancer was a thread within a larger context of healing summits.
Hay House HEAL Summit hosted a seven-day summit with each day covering a healing topic related to the body, heart, emotions, mind, energy, spirit, and the sharing of miraculous healing stories. Thought leaders addressed cancer as part of a topic.
- Kelly Turner, PhD, a best-selling author, researcher, and consultant in the field of integrative oncology, addressed common threads that she has studied on healing mindsets and cancer.
- Veronique Desaulniers, DC, The Breast Cancer Conqueror®, spoke about seven lifestyle changes to beat cancer.
- Siegel, MD, a world-renowned expert in cancer treatment and holistic medicine, addressed healing emotions and how childhood trauma can lead to illness if unaddressed.
- Joe Dispenza, DC, New York Timesbest-selling author, researcher, and international lecturer, discussed his latest findings from the fields of neuroscience, epigenetics and quantum physics to explore the science behind spontaneous remissions. He addressed how this knowledge can help people heal who are experiencing illnesses, chronic conditions, and even terminal diseases—so they can live a more fulfilled and happy life and evolve their level of conscious awareness.
The Embodiment Conference hosted 1,000 speakers over 10 subjects, which ran simultaneously and reached an audience of 500,000.
- Doctors, practitioners, and the general public came together in these sessions and discussions.
- Simultaneous topic channels included Meditation & Breath, Yoga, Coaching & Therapy, Dance & Creativity, Ecology & Research, Intimacy & Relationship, Leadership & Business, Martial & Healing Arts, Movement & Anatomy, and Trauma & Social Change.
- Cancer and many other chronic illnesses were addressed as part of the greater topic.
Love & Resilience: The Contemplative Care Summit
New York Zen Center’s Contemplative Care Programs have transformed the lives of individuals around the world by supporting the integration of spiritual practice and caregiving. Over the past decade of engagement in healthcare environments, New York Zen Center witnessed an acute need for an approach to care that extends beyond the patient and their loved ones to include the clinicians themselves. Too often, and as seen during COVID, clinicians experience burnout, a sense of isolation, and loss of meaning in their work and lives. Now, more than ever, there is a critical need for deeper connections with patients, team members and loved ones in this time of the pandemic.
- Thirty-two presenters focused on themes such as Loving Relationships, Livelihood & Work, Illness & Aging, Death & Dying, and Ritual & Imagination.
- Sensei Koshin Paley Ellison and Sensei Chodo Robert Campbell discussed the transformative and practical aspects of contemplative caregiving.
TREND 4: Yoga and oncology continue to be a priority in clinical research.
Yoga has increasingly become recognized as a complementary approach to reducing the onset and severity of cancer-related symptoms and/or symptom management.
- Individuals are likely to approach yoga as a complementary therapy option based on recommendations from their healthcare team.
- Individuals use yoga to enhance recovery and wellness.
- The underlying reasons for the use of yoga among cancer patients and survivors include relaxing; coping with cancer-related distress, pain and fatigue; taking an active and positive role in their cancer recovery; managing other non-cancer conditions (cardiovascular, disease, arthritis); and increasing energy, physical activity, immunity, sleep and mental cognitive abilities.
Clinical research has demonstrated the acceptability and feasibility of yoga among cancer patients during cancer treatment and after transitioning outside a medical setting.
- 89% of US National Cancer Institute’s (NCI) accredited comprehensive cancer centers provide information on yoga, and 69% offer on-site yoga.
- This rise in information and access to yoga, breathwork and meditation is becoming more present in cancer centers around the globe.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6541520/
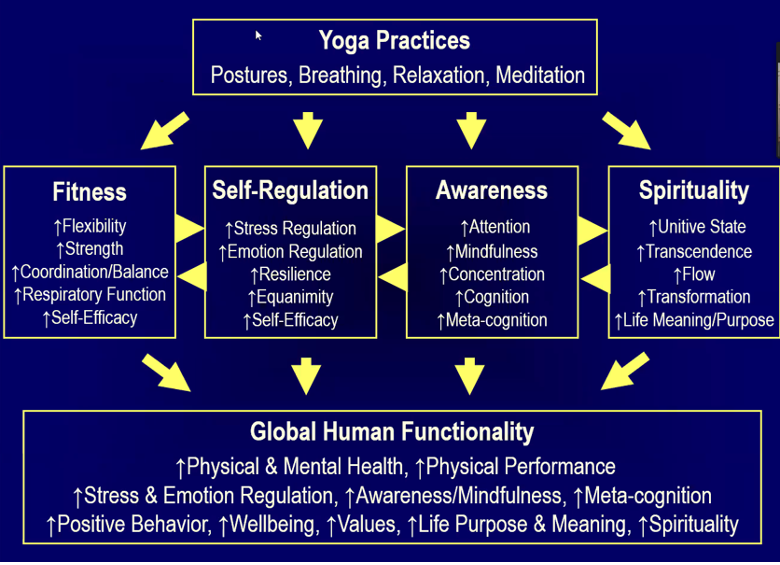 Source: Yoga Alliance on the Evidence of Yoga and Cancer
Source: Yoga Alliance on the Evidence of Yoga and Cancer
TREND 5: Unleashing the power of the immune system as a smart way to prevent, control and eliminate cancer continues to make strides.
Compounding the fear of cancer is the fact that cancer’s treatment is often considered worse than the disease itself. But due to decades of research, cancer immunotherapy (also known as immune-oncology) includes medical treatments designed to harness the power of one’s own immune system to prevent, control and fight cancer.
Immunotherapy enhances the ability of the individual’s immune system to recognize, target and eliminate cancer cells, wherever they are in the body, making it a potential universal answer to cancer.
- The immune system is precise, so it is possible for it to target cancer cells exclusively while sparing healthy cells.
- The immune system can adapt continuously and dynamically, just like cancer does. If a tumor manages to escape detection, the immune system can re-evaluate and launch a new attack.
- The immune system’s “memory” allows it to remember what cancer cells look like, so it can target and eliminate cancer if it returns. This “immuno-memory” may result in longer-lasting and potentially permanent protection against cancer recurrence.
Harnessing the power of the immune system treats the patient, not the tumor. And many believe that it may be reasonable to start using the other “C” word—CURE—to describe the future of cancer.
Source: https://www.cancerresearch.org/
The post Wellness for Cancer Initiative Trends for 2021 appeared first on Global Wellness Institute.
]]>